Insulin has been taking quite a beating these days.
If we’re to listen to some “experts,” it’s an evil hormone whose sole goal is making us fat, type 2 diabetics.
Furthermore, we’re told that carbohydrates also are in on the conspiracy. By eating carbs, we open the insulin floodgates and wreak havoc in our bodies.
How true are these claims, though? Does it really make sense that our bodies would come with an insidious mechanism to punish carbohydrate intake?
Let’s find out.
What is Insulin, Anyway?
Insulin is a hormone, which means it’s a substance the body produces to affect the functions of organs or tissues, and it’s made and released into the blood by the pancreas.
Insulin’s job is a very important one: when you eat food, it’s broken down into basic nutrients (protein breaks down into amino acids; dietary fats into fatty acids; and carbohydrates into glucose), which make their way into the bloodstream.
These nutrients must then be moved from the blood into muscle and fat cells for use or storage, and that’s where insulin comes into play: it helps shuttle the nutrients into cells by “telling” the cells to open up and absorb them.
So, whenever you eat food, your pancreas releases insulin into the blood. As the nutrients are slowly absorbed into cells, insulin levels drop, until finally all the nutrients are absorbed, and insulin levels then remain steady at a low, “baseline” level.
This cycle occurs every time you eat food: amino acids, fatty acids, and/or glucose find their way into your blood, and they’re joined by additional insulin, which ushers them into cells. Once the job is done, insulin levels drop to “normal” and the pancreas waits for us to eat food again and repeat the process.
What’s the Problem With Insulin, Then?
When explained like that, insulin sounds like an alright dude. We can’t live without it.
Why, then, is it viciously attacked by mainstream diet “gurus”? Why are we told it makes us fat and sick?
Because one of insulin’s vital roles in the body relates to fat storage: it inhibits the breakdown of fat cells and stimulates the creation of body fat. That is, insulin tells the body to stop burning its fat stores and instead, absorb some of the fatty acids and glucose in the blood and turn them into more body fat.
This makes it an easy target and scapegoat, and this is why the carbohydrate is often pilloried right next to it. The “logic” goes like this:
High-carb diet = high insulin levels = burn less fat and store more = get fatter and fatter
And then, as a corollary:
Low-carb diet = low insulin levels = burn more fat and store less = stay lean
At first glance, these statements sound plausible. Simple explanations are popular.
But they’re based on myths and pseudoscience.
Insulin Triggers Fat Storage…But It Doesn’t Make You Fat
One of the common charges against carbohydrates and insulin is that by eating a lot of carbs every day, your insulin levels will remain chronically high. This, in turn, (supposedly) causes weight gain because your body will constantly be in “fat storage mode” and rarely in “fat burning mode.”
It sounds good, but it’s a myth.
It’s true that insulin causes fat cells to absorb fatty acids and glucose and thus expand, but that’s not what causes you to get fatter over time…overeating does. (Click here to tweet this!)
If that doesn’t make sense to you, let’s quickly review how energy balance relates to fat gain and loss. Energy balance refers to the amount of energy you burn every day versus the amount you give your body via food.
- If you give your body a bit more energy than it burns every day, a portion of the excess energy is stored as body fat, and thus you gain weight slowly
- If you give your body a bit less energy than it burns every day, it will tap into fat stores to get the additional energy it needs, and thus you lose weight slowly
You see, any any given time, your body requires a certain amount of glucose in the blood to stay alive. This is vital fuel that every cell in the body uses to operate, and certain organs like the brain are real glucose hogs.
Now, when you eat food, you give your body a relatively large amount of energy (calories) in a short period of time. Glucose levels rise far above what is needed to maintain life, and instead of “throwing away” or burning off all excess energy, a portion is stored as body fat for later use.
Scientifically speaking, when your body is absorbing nutrients eaten and storing fat, it’s in the “postprandial” state (post meaning “after” and prandial meaning “having to do with a meal”). This “fed” state is when the body is in “fat storage mode.”
Once the body has finished absorbing the glucose and other nutrients from the food (amino acids and fatty acids), it then enters the “postabsorptive” state (“after absorption”), wherein it must turn to its fat stores for energy. This “fasted” state is when the body is in “fat burning mode.”
Your body flips between “fed” and “fasted” states every day, storing fat from food you eat, and then burning it once there’s nothing left to use from the meals. Here’s a simple graph from Weightology that shows this visually:
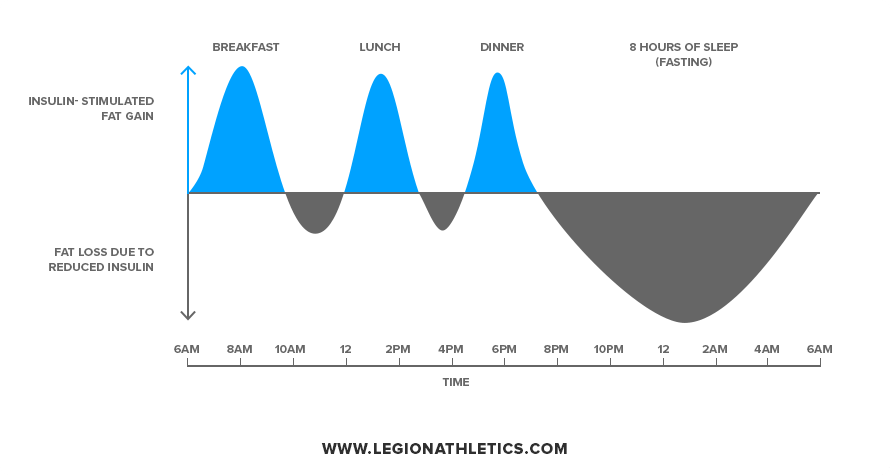
The blue portions are the periods where your body has excess energy due to food having been eaten. The gray portions are the periods when the body has no energy left from food and thus has to burn fat to stay alive.
If the blue and gray portions balance out every day–if you store just as much fat as you burn–your weight stays the same. If you store more fat than you burn (by overeating), you get fatter. And if you burn more fat than you store, you get leaner.
This is the fundamental mechanism underlying fat storage and fat loss and it takes precedence over anything related to insulin or any other hormones in the body.
Simply put, you can’t get fatter unless you feed your body more energy than it burns, and you can’t get leaner unless you feed it less energy than it burns.
It doesn’t matter how many carbohydrates you eat or how high your insulin levels are throughout the day–this is the first law of thermodynamics at work. Fat stores can’t be increased without the provision of excess energy, nor can they be reduced without the restriction of energy.
That’s why research has shown that so long as they’re eating less energy than they’re burning, people lose fat equally well on high-carbohydrate or low-carbohydrate diets. That’s why professor Mark Haub was able to lose 27 pounds on a “convenience store diet” consisting mainly of Twinkies, Little Debbie cakes, Doritos, and Oreos: he simply fed his body less energy than it was burning.
(And if you feel confused about how many calories, how much of each macronutrient, and which foods you should eat to reach your weight-loss goals, take the Legion Diet Quiz to learn exactly what diet is right for you.)
The bottom line is your insulin levels and the amount of carbs you eat have little to do with losing or gaining weight–energy balance is the key.
(If you want to know more about carbohydrates and weight loss, and when low-carb dieting is actually better, check out this article.)
Insulin Isn’t the Only Substance That Triggers Fat Storage
You already know that insulin causes fat cells to absorb glucose and fatty acids. Well, there’s another reason it’s charged with causing weight gain.
Your fat cells contain an enzyme called hormone-sensitive lipase (HSL), which helps break down body fat into fatty acids to be burned. Insulin suppresses the activity of HSL, and thus is believed to further promote weight gain.
Well, something carb- and insulin-haters like to ignore is the fact that dietary fat also suppresses HSL, and thanks to an enzyme called acylation stimulating protein, your body doesn’t need high levels of insulin to store dietary fat as body fat.
This is why you can’t just eat as much dietary fat as you want and lose weight. And why research has shown that separating carbs and fats doesn’t affect weight loss (eating carbs and fats together or separately doesn’t change anything).
Once again, it comes back to energy balance–regularly give your body more energy than it burns, whether in the form of protein, carbohydrate, or fat, and you’ll get fatter.
Protein Stimulates Insulin Production Too
This is another fact low-carb “gurus” like to avoid.
High-protein, low-carbohydrate meals can cause more insulin to be released than high-carbohydrate meals. Whey protein in particular has been shown to be more insulinogenic than white bread. Beef stimulates just as much insulin release as brown rice.
And in case you think the insulin response to protein is more moderate and prolonged (as if this were somehow better), it’s not–protein causes a rapid rise in insulin followed by a rapid decline, just like carbs.
Ironically, a high-protein, high-fat meal causes more immediate fat storage than a high-carbohydrate meal because dietary fats are stored very efficiently as body fat.
Insulin Doesn’t Stimulate Hunger–It Does the Opposite
This is another myth bandied about, but it’s been disproved by clinical research.
In fact, research has demonstrated that the more insulinogenic a meal, the more full you feel as a result. This correlates with research demonstrating that high-carbohydrate meals induce more satiety (fullness) than high-fat meals.
Insulin Helps You Build Muscle
While insulin doesn’t directly induce protein synthesis like amino acids do, it does have anti-catabolic properties.
What that means is when insulin levels are elevated, the rate at which muscle proteins are broken down decreases. This, in turn, creates a more anabolic environment in which muscles can grow larger quicker.
That sounds good in theory, right? But does it pan in out clinical research? Yes, it does.
There are several studies that conclusively show that high-carbohydrate diets are superior to low-carbohydrate varieties for building muscle and strength.
Researchers at Ball State University found that low muscle glycogen levels (which is inevitable with low-carbohydrate dieting) impair post-workout cell signaling related to muscle growth.
A study conducted by researchers at the University of North Carolina found that when combined with daily exercise, a low-carbohydrate diet increased resting cortisol levels and decreased free testosterone levels. (Cortisol, by the way, is a hormone that breaks tissues, including muscle, down. In terms of maximizing muscle growth, you want low resting cortisol levels and high free testosterone levels.)
These studies help explain the findings of other research on low-carbohydrate dieting.
For example, a study conducted by researchers at the University of Rhode Island looked at how low- and high-carbohydrate intakes affected exercise-induced muscle damage, strength recovery, and whole body protein metabolism after a strenuous workout.
The result was the subjects on the low-carbohydrate diet (which wasn’t all that low, actually—about 226 grams per day, versus 353 grams per day for the high-carbohydrate group) lost more strength, recovered slower, and showed lower levels of protein synthesis.
In this study, researchers at McMaster University compared high- and low-carbohydrate dieting with subjects performing daily leg workouts. They found that those on the low-carbohydrate diet experienced higher rates of protein breakdown and lower rates of protein synthesis, resulting in less overall muscle growth than their higher-carbohydrate counterparts.
All this is why I never drop my carbohydrate intake lower than about .8 grams per pound of body weight when cutting (and yes I get to 6% body fat eating this many carbs per day), and I’ll go as high as 2 to 2.5 grams per pound when bulking.
Insulin Isn’t the Problem…Being Overweight and Sedentary Is
The bottom line with carbohydrate intake and insulin levels is this:
If you’re overweight and sedentary, regular intake of large amounts of carbohydrates is going to cause problems in the long run. Your body is going to have more and more trouble dealing with insulin, which can, over time, even develop into Type 2 diabetes, and you’re going to be at greater risk for heart disease.
If you stay lean, exercise regularly, and eat at least a reasonably sensible diet, you’ll never have these problems. You’ll maintain insulin sensitivity and your body will have plenty of use for the carbs you eat.










