I’ve long preferred biking to running but a few months back decided to mix things up…and I quickly learned how much shin splints suck.
The pain would come on fast and hard, like a vise clamping down on my leg, and the more I ran, the worse it got.
That, of course, got me wondering. What are shin splints? What causes them? And what can I do to treat and prevent such an aggravating pain?
Well, I read up, tried various strategies, and want to share with you what I’ve learned.
So let’s get to it.
What Are Shin Splints?
Shin splints is the layman’s way to refer to what’s known medically as medial tibial stress syndrome (MTSS).
And while they might feel like fiery demons are waging war against your shins, the common causes are far less exciting.
There are two primary causes for shin splints: excessive pressure and/or impact on the lower leg tissues and bone.
Simply put, when the tibial muscles, tendons and bone tissue becomes overworked, the pain begins. And the more you try to push through it, the worse it gets.
There are two types of shin splints: anterior and posterior. Anterior shin splints are felt down the front of the leg and posterior are felt down the inside of the leg.
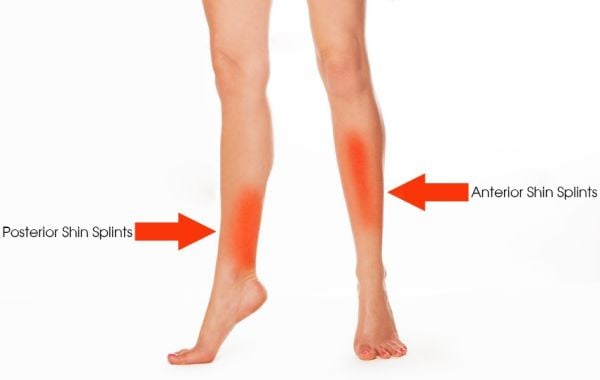
Not all shin pain is caused by shin splints, though.
Pain on the outside of the lower leg might be compartment syndrome, which is a buildup of pressure in a section of the body that contains muscles and nerves. Symptoms of compartment syndrome include pain, strange nerve sensations, and muscle weakness.
Stress fractures (small fractures) are often mistaken for shin splints and may even accompany them.
A bone scan is necessary to know for certain, but one way to tell shin splints from stress fractures is to run your fingers over your shin, applying pressure. If you find a spot that triggers sharp pain, that’s a sign of a stress fracture. Shin splint pain is more generalized.
Stress fractures also tend to feel better in the morning, after the bone has rested all night, whereas shin splints often feel worse when you wake up because the inflamed tissues tighten overnight. Shin splints also flare up when you flex your foot up or down, depending on which tibial muscle is aggravated.
Ultimately, there isn’t a consensus among sport scientists as to exactly what’s causing the shin splint pain. Theories include inflammation of and/or small tears in the tibial muscles, inflammation of the periosteum (a thin layer of tissue wrapping around the bone), damage to the bone itself, and various combinations of these.
Fortunately, however, common causes and effective treatments and preventative measures are better understood.
What Are the Common Causes of Shin Splints?

Any runner will tell you that shin splints tend to begin when mileage is increased or running surface hardens or terrain changes (hill running is a common trigger).
Other common causes are worn-out footwear, overpronation, flat feet, and even excessive stress placed on one side of the body from running on cambered roads or always in the same direction on a track.
It’s not the exercise per se that causes the problems, though; it’s the repeated shocks of landing and changing directions that does it.
This fatigues and overloads the muscles of the lower leg, which makes them less and less able to absorb the force of the blows. This is why shin splints only get worse if you try to push through them.
The common causes of shin splints can be boiled down to this: too much, too fast. This, then, informs how to properly treat them…
How to Get Rid of Shin Splints

Like any exercise-related injury, the first thing you have to do when you get shin splints is, depending on the severity, decrease or stop whatever is causing the problem.
The general recommendation is 2 to 6 weeks of rest, but that doesn’t mean you have to stop training completely.
For example, if running on a very hard surface like concrete ignites your shins, switching to a softer surface like pavement, gravel, dirt, or grass, can be enough to provide relief. You should also avoid hills and uneven surfaces.
Many people find that shin splints come on after several miles of running, or after several runs in a week. In these cases, reducing the length or frequency of the runs is likely to help.
If any amount of running whatsoever is a problem, you can switch to biking or swimming or some other form of cardio that doesn’t cause you pain.
You also want to start icing your shins every day to reduce inflammation. The easiest way to do this is with a special ice pack like this:
And to follow a standard RICE protocol of 10 to 20 minutes of ice 3 or more times per day.
There are two stretches that can help as well.
1. Stretching your calves and Achilles tendons.
2. Stretching your shins.
There’s evidence that other therapies can help such as deep tissue massage and acupuncture, but the research is inconclusive. If you have the money, time, and inclination, there’s no harm in trying them.
The Bottom Line on Getting Rid of Shin Splints
As you can see, patience is a big part of treating shin splints.
The strategies given above can speed the healing process up, but you can still expect 2 to 6 weeks of recovery time until the pain goes away, and it’s very important that you make sure you’re pain-free before you resume your normal activities.
How to Prevent Shin Splints

I’m of the mind that treatments are good but prevention is better. Why wait to fix something that’s broken when you can keep it from breaking in the first place?
Well, many people struggle with shin splints on and off for years without realizing there are ways to prevent them.
We’ll discuss the scientifically validated methods here.
Strengthen Your Core, Glutes, and Calves and Shin Muscles
Developing these muscles can improve running mechanics and prevent overuse injuries like shin splints.
Here are workouts that can help you with the major muscle groups:
The Ultimate Ab Workouts: The 5 Best Ab Exercises for Getting a Six Pack
The Best Butt Exercises for Building Head-Turning Glutes
The Ultimate Calves Workouts for Quickly Adding Size and Strength
And here are a few simple exercises for strengthening your shin muscles:
Stop Heel Striking
“Heel striking” is just what it sounds like it–landing heels-first when you run.
The impact of the heel strike is significantly worse than a proper midfoot landing, which is why heel striking is known to increase the risk of developing shin splints and other running-related injuries.
Here’s a good video that shows the difference between heel striking and midfoot running:
If you want to learn more about how to run properly, prevent injury, and maximize enjoyment and performance, check out Kelly Starrett’s latest book Ready to Run:
Use the Right Shoes
Worn-out and/or ill-fitting shoes can contribute to shin splints and, contrary to popular belief, soft, cushiony shoes can as well.
Shock absorption is part of the reason why shoes matter but stability is equally if not more important.
Overpronation is extremely common and you want your shoes to help prevent it. And in case you’re not familiar with overpronation, here’s what it looks like:
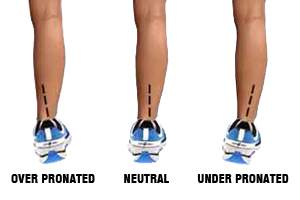
As you can see, when the ankles roll too much to the inside, they’re overpronated, and this puts extra pressure on your shins.
Well, good running shoes can help this whereas battered or squishy shoes or ones that don’t fit can’t.
This is one of the reasons why it’s generally recommended that you replace your running shoes every 200 to 300 miles (and that you never wait longer than 500 miles).
I’m not big on running so don’t have much in the way of personal recommendations for shoes, but I would go with something made to prevent overpronation and promote midfoot strikes, like one of these:
What About Compression Socks?
Compression socks (and compression gear in general) is popular among athletes and there’s good evidence that it can help reduce muscle soreness and speed muscle recovery.
Thus, it’s understandable why compression socks are commonly recommended for preventing shin splints, but research casts doubt on this application.
That said, studies on compression socks are all over the place and hard to interpret due to the wide range of socks used, the experience level of the runners involved, and the inability to accurately measure certain parameters.
Remember that when we’re talking health, fitness, and exercise, anecdotal evidence can be valuable, and especially where scientific evidence is conflicting or meager.
If I were struggling with shin splints, I’d give compression socks a go because enough people say it gives them relief. I’d chalk it up to “worth a shot.”
And if you’re going to do that, you should know that research suggests that there is a “sweet spot” for the amount of compression provided by the sock. In this study, scientists found that, in subjects at rest, 20mmHg at the ankle improved blood flood but 30mmHg restricted it.
Furthermore, graduated compression is most effective, which means you want a sock that is tighter in the ankle are than the knee.
Here’s a compression sock from a reputable brand (CEP) that meets these criteria:
Or you could go with their compression sleeve if you prefer:
And in terms of how to use compression socks/sleeves, you can run with them and/or wear them afterward. Many people wear them as much as they can tolerate, which seems to range from several to 16+ hours. Experiment and see how your body responds.
If wearing them for long periods of time causes pain, though, it’s time to take them off. The compression can eventually aggravate baroreceptors in your leg, which is going to hurt.
The Bottom Line on Shin Splints

As debilitating as your shin splints might be, you can get rid of them for good, and this article shows you how.
If you’re currently in the throes of tibial torture, back off and let them heal, and then strengthen your core and lower body, work on your running technique, make sure your shoes are up to snuff, and if you’re willing to give them a go, pick up some high-quality compression socks.
Happy running!
What’s your take on shin splints? Have anything else to share? Let me know in the comments below!
Scientific References +
- Byrne B. Deep vein thrombosis prophylaxis: The effectiveness and implications of using below-knee or thigh-length graduated compression stockings. Hear Lung J Acute Crit Care. 2001;30(4):277-284. doi:10.1067/mhl.2001.116009
- Moen MH, Holtslag L, Bakker E, et al. The treatment of medial tibial stress syndrome in athletes; a randomized clinical trial. Sport Med Arthrosc Rehabil Ther Technol. 2012;4(1). doi:10.1186/1758-2555-4-12
- Hill J, Howatson G, van Someren K, Leeder J, Pedlar C. Compression garments and recovery from exercise-induced muscle damage: a meta-analysis. Br J Sports Med. 2014;48(18):1340-1346. doi:10.1136/bjsports-2013-092456
- Born DP, Sperlich B, Holmberg HC. Bringing light into the dark: Effects of compression clothing on performance and recovery. Int J Sports Physiol Perform. 2013;8(1):4-18. doi:10.1123/ijspp.8.1.4
- Hatala KG, Dingwall HL, Wunderlich RE, Richmond BG. Variation in Foot Strike Patterns during Running among Habitually Barefoot Populations. Lucia A, ed. PLoS One. 2013;8(1):e52548. doi:10.1371/journal.pone.0052548
- Niemuth PE, Johnson RJ, Myers MJ, Thieman TJ. Hip muscle weakness and overuse injuries in recreational runners. Clin J Sport Med. 2005;15(1):14-21. doi:10.1097/00042752-200501000-00004
- Wilder RP, Sethi S. Overuse injuries: Tendinopathies, stress fractures, compartment syndrome, and shin splints. Clin Sports Med. 2004;23(1):55-81. doi:10.1016/S0278-5919(03)00085-1
- Beck BR. Tibial stress injuries. An aetiological review for the purposes of guiding management. Sport Med. 1998;26(4):265-279. doi:10.2165/00007256-199826040-00005
- Couture CJ, Karlson KA. Tibial stress injuries: Decisive diagnosis and treatment of “shin splints.” Phys Sportsmed. 2002;30(6):29-36. doi:10.3810/psm.2002.06.337
- Galbraith RM, Lavallee ME. Medial tibial stress syndrome: Conservative treatment options. Curr Rev Musculoskelet Med. 2009;2(3):127-133. doi:10.1007/s12178-009-9055-6
- Thacker SB, Gilchrist J, Stroup DF, Kimsey CD. The prevention of shin splints in sports: A systematic review of literature. Med Sci Sports Exerc. 2002;34(1):32-40. doi:10.1097/00005768-200201000-00006