Key Takeaways
- Knee pain is poorly understood, and many of the things that people think help either aren’t scientifically supported or have been debunked.
- Unless you’ve damaged your knee in some kind of accident, then the most likely cause of knee pain is overuse—doing too much with too little rest.
- The only reliable way to reduce most kinds of knee pain is to rest until your knee is completely pain free, although there are seven other strategies that may help as well.
Healthy, pain-free knees are one of those things you don’t appreciate until they’re gone.
When your knees start hurting, your favorite exercises become excruciating, you’re forced to use lighter and lighter weights, and everyday activities become a source of constant torment.
Knee pain is also insidious.
It starts out small—just enough to annoy you but not enough to make you stop whatever you’re doing—and then it grows and grows until it becomes a constant nuisance.
It usually goes something like this:
Your knees feel tight for a moment during a workout.
You shrug it off and keep going. It isn’t really pain, more just discomfort, and you’re confident it will go away in a day or two.
But it doesn’t.
During your next workout, that “tightness” transforms into brief, shooting pains, especially when you bend your knee.
You make it through a few more workouts before you realize this problem isn’t going away any time soon.
Fast forward several weeks, and now your knees hurt all of the time, even when you aren’t working out.
You’re stuck in knee pain purgatory.
You can’t train hard enough to get stronger, but you keep training hard enough to prevent your knees from healing.
In desperation you ask your friends what to do, and everyone has a different opinion.
Most people immediately recommend surgery. “Someone’s going to have to go in there and clean it out,” they say, as if bad knees just need an oil change.
Others will tell you that this is the price you pay for lifting heavy weights. What did you expect would happen from squatting, lunging, and deadlifting every week?
And others will say that your knee pain can easily be solved by fixing your posture, technique, and muscle imbalances. It’s all caused by the way you move, they say.
The solutions you find online leave you even more confused. Here’s just a short list of the things people say you should try:
- Surgery
- Stretching
- Massage
- Chiropractic
- Foam rolling
- Acupuncture
- Prolotherapy injections
- Posture correction
- NSAIDs
- Glucosamine chondroitin
- Ice
- Yoga
- Physical therapy
- Transcutaneous Electrical Nerve Stimulation (TENS)
- Corticosteroid injections
. . . and more.
There’s a reason everyone seems to have an opinion. One in four adults suffers from knee pain at some point in their lives, and it’s even more endemic in athletes.
So, how are you supposed to know who’s right?
Well, the short story is this:
Knee pain is a poorly understood phenomenon, and outside of a few rare cases, it’s almost impossible to tell exactly what’s causing it. The good news, though, is that most forms of knee pain resolve by themselves if you rest properly (and that’s not as simple as just staying out of the gym).
In this article, you’ll learn what causes knee pain, what does and doesn’t work for reducing knee pain, and the seven best ways to fix knee pain for good.
Let’s get started.
What Causes Knee Pain?
Before we get into what causes knee pain, we need to understand the basic anatomy of the knee joint.
The knee’s job is to allow the lower leg to flex while stabilizing the femur.
It’s one of the best examples of a hinge joint in the body, which means the knee only moves in a single plane (forward and backward).
The main structures of the knee include:
- The femur (thigh bone)
- The tibia (shin bone)
- The patella (kneecap)
- The patellar tendon
- The medial meniscus
There are also a collection of ligaments, smaller tendons, and fluid-filled sacs called bursa that act as padding between tendons and bones. The entire joint is surrounded in synovial fluid, which is a goo about the consistency of egg whites that lubricates the cartilage in joints.
Here’s what all of this looks like from the front:
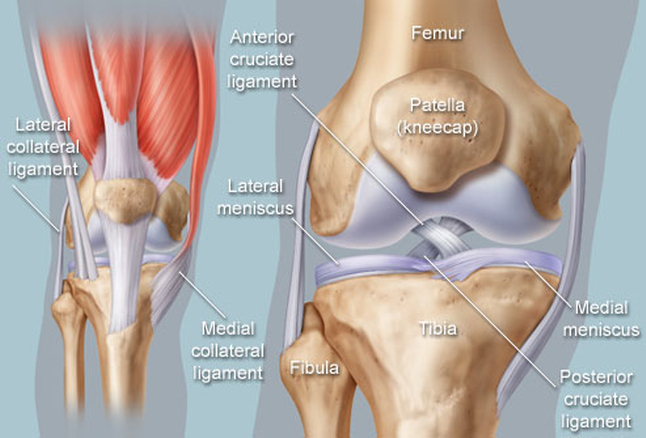
And from the side:
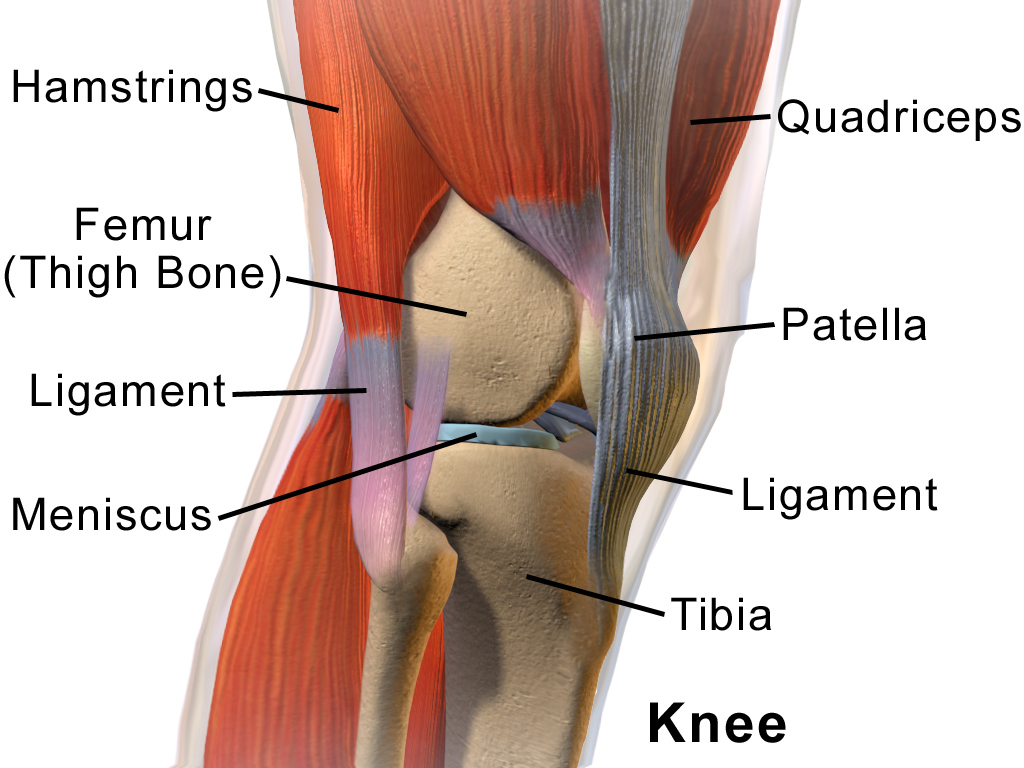
Several other structures also affect the knee, including the muscles of the upper leg (the quadriceps and hamstrings) and the iliotibial band, which is a large piece of connective tissue that extends down the side of each leg and across the knee. Here’s what it looks like:
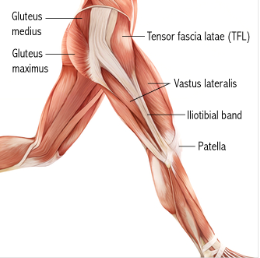
There are three main kinds of knee injuries:
- Repetitive strain injuries (RSIs).
- Traumatic injuries.
- Chronic injuries.
Let’s look at each.
1. Repetitive strain injuries (RSIs).
Repetitive strain injuries are caused by the wear and tear from repeated movement and overuse.
RSIs tend to start small and get progressively worse over time, which leads many people to keep training and make the problem much worse before it gets better.
Some of the most common knee RSIs include . . .
- Patellofemoral pain syndrome
- Patellar tendonitis
- Inflammation of the bursa (bursitis)
- Degeneration of the tendons (tendinosis)
- Degeneration of cartilage (chondromalacia)
Most kinds of unexplained, sudden knee pain are linked to RSIs. This is because they tend to slowly get worse over time, until one day, the knee starts hurting for seemingly no reason.
The truth, of course, is that the knee probably endured weeks or months of abuse until it couldn’t take it any more and started hurting.
RSIs are one of the most common causes of knee pain in athletes, and luckily, they’re also the easiest to fix.
2. Traumatic injuries.
Traumatic injuries are injuries caused by an immediate tear, strain, or bruise.
When it comes to knee pain, this would be something like letting one of your knees cave inward when squatting or landing on your knee at a strange angle during a football game, like this:
Most traumatic knee injuries are caused by car accidents or playing sports, but it’s not uncommon for people to hurt their knees from every day activities or accidents, like slipping on ice.
Some of the most common traumatic injuries include . . .
- Meniscal tear
- Anterior cruciate ligament (ACL) tears
- Posterior cruciate ligament (PCL) tears
- Medial cruciate ligament (MCL) tears
- Patellar fracture
- Patellar tendon tear
Luckily, these kinds of injuries are relatively rare. When they do happen, they’re usually painful enough that people have the common sense not to keep training, too.
Some of these injuries are relatively easy to fix (like a small patellar fracture, which usually heals on its own), while others might never fully heal, (like a complete ACL rupture).
If you’ve had a traumatic injury and you’re sure that’s what’s causing your knee pain, then you’re better off seeing a doctor. There isn’t much you can do on your own, which is why this article is mostly about repetitive strain injuries and chronic injuries.
3. Chronic injuries.
Chronic injuries are any kind of repetitive strain or traumatic injury that should have healed, but hasn’t.
In most cases, these kinds of injuries only bother you off and on, and while they’re painful enough to be annoying, they aren’t bothersome enough to make you stay out of the gym.
Chronic injuries can be caused by any number of things, but as you’ll see, they’re typically related to overuse.
By far the most common of these three injuries is the repetitive strain injury.
That doesn’t tell us what’s hurting, why it’s hurting, or what to do about it, though.
And unfortunately, it’s impossible to find definitive answers to those questions.
Muscle pain and tightness are rather mysterious phenomena, and many of things that have long been assumed to cause them have been debunked.
For instance, many people think that any kind of knee pain must be caused by inflammation of the muscle, bursa, or tendon (such as tendonitis) but the truth is that many knee injuries aren’t inflamed.
Instead, there are tiny microtears in the joint structures that your body hasn’t been able to repair as fast as you’ve been creating them, which compromises the strength of those tissues (this is known as tendinosis).
This is why physical therapists often give people several different treatments, in the hopes that one or some of them will work. As unscientific as it sounds, reducing pain is often a matter of throwing a bunch of solutions at the wall and seeing what sticks.
Many studies do the same thing, which is why research on pain science can be so misleading.
For example, a study might compare a group of people who do a structured warm-up, physical therapy, and foam rolling to a group that doesn’t do anything. Sure enough, the group that tries all of the new techniques gets fewer injuries.
Then, people will point to that study as proof that foam rolling works, when there’s no way to tell which method really moved the needle.
That said, you still want to focus on the things that are likely to work, so let’s look at some of the most common things people use to fix knee pain and see how they stack up.
What’s the Best Way to Reduce Knee Pain?
Here’s the bad news: There’s very little research on the best ways to reduce knee pain, specifically.
Most of the studies that we do have are about surgery for traumatic knee injuries (like ligament tears) or treatments for rheumatoid arthritis, which is an autoimmune disease wherein the body’s immune system attacks its own joint cartilage.
That research isn’t very helpful for us fitness folk, who just want to be able to get back in the gym without knee pain.
The good news?
There’s a lot of data on pain and joint pain in general, and it’s fair to assume that most of that applies to knee pain, too.
With that in mind, let’s look at 19 of the best and worst cures for knee pain, and see how they stack up against the evidence.
Knee Pain and Surgery
Tell someone you’re having knee pain, and the vast majority will assume it’s caused by damage to the cartilage in your knee. Specifically, knee pain is usually blamed on a meniscal tear, or a tear in the meniscus of the knee.
The meniscus is a crescent-shaped piece of cartilage that acts as a cushion between the femur and the tibia. There’s a medial and lateral meniscus, and they look like this:
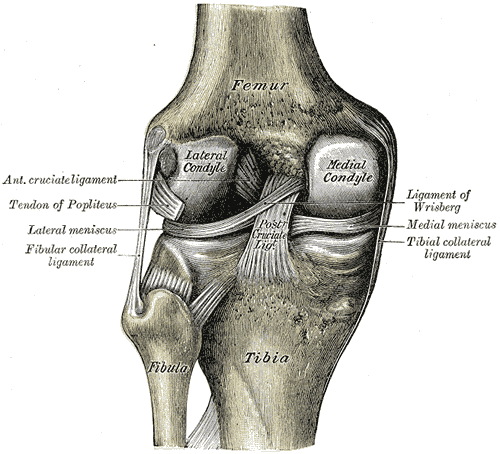
It’s a well-known fact that the meniscus, like most of the cartilage in joints, doesn’t heal quickly. Compared to other tissues like muscle and skin, cartilage has very few blood vessels and thus doesn’t regenerate as fast.
It’s incredibly tough stuff, but if it does get damaged that wear and tear tends to take much longer to heal than other injuries.
This is why so many doctors, trainers, and physical therapists recommend surgery almost without question if you say that your knees hurt.
If your body isn’t going to fix the problem, then a surgeon’s going to have to go in there and do it for you.
The most common surgery for fixing damaged joint cartilage is known as “debridement,” which entails filing down or clipping away rough knee cartilage to create a smooth surface. Theoretically, these jagged edges of torn joint cartilage interfere with the knee’s natural movement, and cutting them out should reduce pain and improve knee function.
And it makes sense.
If you envision the human body as a machine, you don’t want jagged parts rubbing against each other. Those plastic models in doctor’s offices are also convincing. Do you really want your joint cartilage to look like this?

Of course not. You want a nice, smooth, knee, so this whole debridement thing sounds great.
And you aren’t the only one who feels that way. There are over 650,000 knee debridement surgeries per year in the U.S., with an average cost of $5,000.
There’s just one problem—it doesn’t work.
This myth was definitively put to rest by a study published in the prestigious New England Journal of Medicine back in 2002. In the study, 180 people were split into two groups. One group received state-of-the-art knee debridement surgery and “lavage,” which involves running water through the knee joint to wash out pieces of cartilage and other particles that might irritate the knee.
The other group was put under anesthesia, cut open, and put through every step that the first group was, with one key difference: the surgeons never actually performed the surgery.
They took tremendous pains to make sure the subjects wouldn’t know, too, like moving the knee in the same way they normally would during surgery, splashing water to mimic the sound of lavage, and asking nurses to hand them surgical tools just as they would during the real procedure.
The result?
There was zero difference in pain, knee function, and stair-climbing ability two weeks after the surgery. The researchers took all of the same measurements again six times over the next two years, and there was still no difference at any point.
Ironically, the group that got the real surgery had slightly worse knee function over the following two years.
The surgery was a complete flop.
This idea has been so thoroughly debunked that the British Medical Journal recommends against it even if there’s obvious damage to the knee or other symptoms of arthritis.
Many other studies have proven the same thing time and time again. Even simple leg exercises show better results than this kind of knee surgery.
This doesn’t mean all kinds of knee surgery are useless, though. For example, reconstructive surgery for ACL injuries can often help people regain excellent knee function.
But when it comes to trying to fix knee pain that’s caused by joint degeneration, overuse, or general wear and tear, surgery is a complete dud.
The bottom line is that the most common form of knee surgery (debridement) doesn’t work. People who get a fake knee surgery consistently do just as well or slightly better than people who get the real surgery, and other solutions like leg-strengthening exercises work much better.
Knee Pain and Muscle Imbalances
Many people believe that knee pain is caused by muscle imbalances.
Ask these people what they mean exactly, and the conversation inevitably leads to what’s known as patellofemoral tracking syndrome.
To understand this argument, we need to cover some more anatomy.
The patella is a bone about the size of a small oyster that’s anchored to the upper leg muscles by the quadriceps tendon, and the tibia (shin bone) by the patellar tendon.
It looks like this:
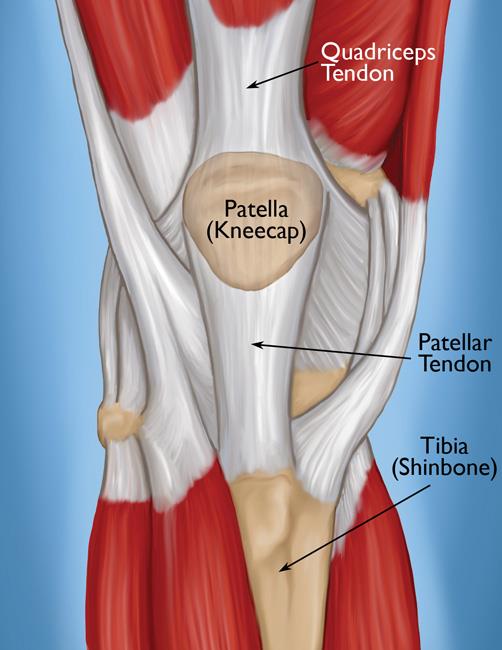
During healthy knee function, the muscles of the upper leg pull on the patella, which causes it to glide, or “track,” over the top of the femur.
This is what it looks like in action:
(The big bone on the left of the screen is the femur).
The idea of patellofemoral tracking syndrome, is that the muscles of the upper leg can pull the patella out of alignment, causing it to slide unevenly along the femur. This makes the patella grind into the femur when you flex and extend your knee, and over time this wears down the cartilage in your knee and causes pain.
If you go to see a physical therapist, personal trainer, or just about any other expert, chances are good they’ll run you through some kind of patellar tracking test. Then, they’ll say that one or more muscles in your leg is weak, and give you a list of exercises to fix the problem.
One muscle in particular gets the lion’s share of the blame—the vastus medialis obliquus (VMO). The VMO is a quadriceps muscle on the inside of your front thigh that’s attached to the patella.
This is what it looks like:
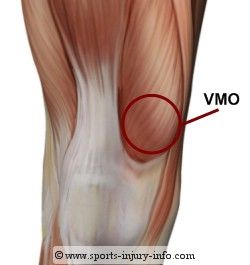
Strengthen this muscle, you’re told, and your patella will start tracking normally again, and the knee pain will go away.
Sounds logical enough, right?
Not quite.
There are several other gaping holes in this logic.
If this were the case, then you’d expect a weak VMO muscle to be associated with more knee pain and patellar dysfunction, but that’s not true.
There’s also no clear definition of what “normal” patellar movement is, and many people’s patellas move in odd ways with no sign of pain or dysfunction. Even trained physical therapists can’t agree on what “normal” patellar tracking should look like.
Strengthening the muscles of the leg can help reduce knee pain, but there’s little evidence that’s because this fixes muscle imbalances, that muscle imbalances caused pain in the first place, or that muscle imbalances affect patellar tracking at all.
The bottom line is that muscle imbalances are very unlikely to cause knee pain, and the strength of specific leg muscles (like the VMO) isn’t linked with patellar tracking or knee pain.
Knee Pain and Stretching
The idea that stretching reduces knee pain goes something like this:
- “Tightness” and lack of flexibility can cause and prolong injuries, so becoming more flexible reduces pain and helps you heal faster.
- Stretching makes you more flexible, so stretching helps fix your knee pain.
When talking about knee pain specifically, you’re normally told to stretch your iliotibial band (IT band).
The iliotibial band is a large piece of connective tissue that runs from the top of your pelvis, down the outside of your hip, to the top of the tibia. It looks like this:
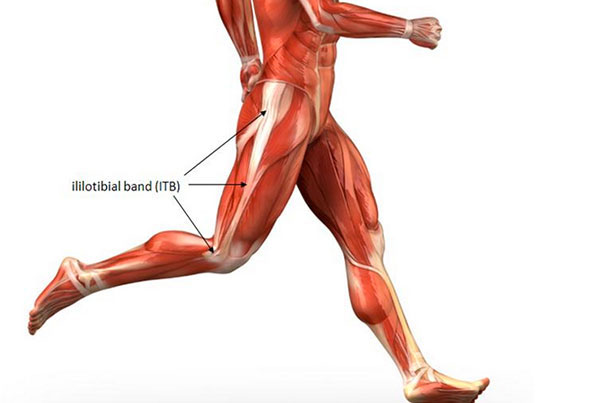
The commonly accepted idea is that the iliotibial band can become tight, and when that happens, it rubs against a bump on the top of the tibia called the lateral epicondyle, which creates pain.
This is why it’s known as iliotibial band friction syndrome.
To fix this, you’re told to stretch your iliotibial band with exercises like this:
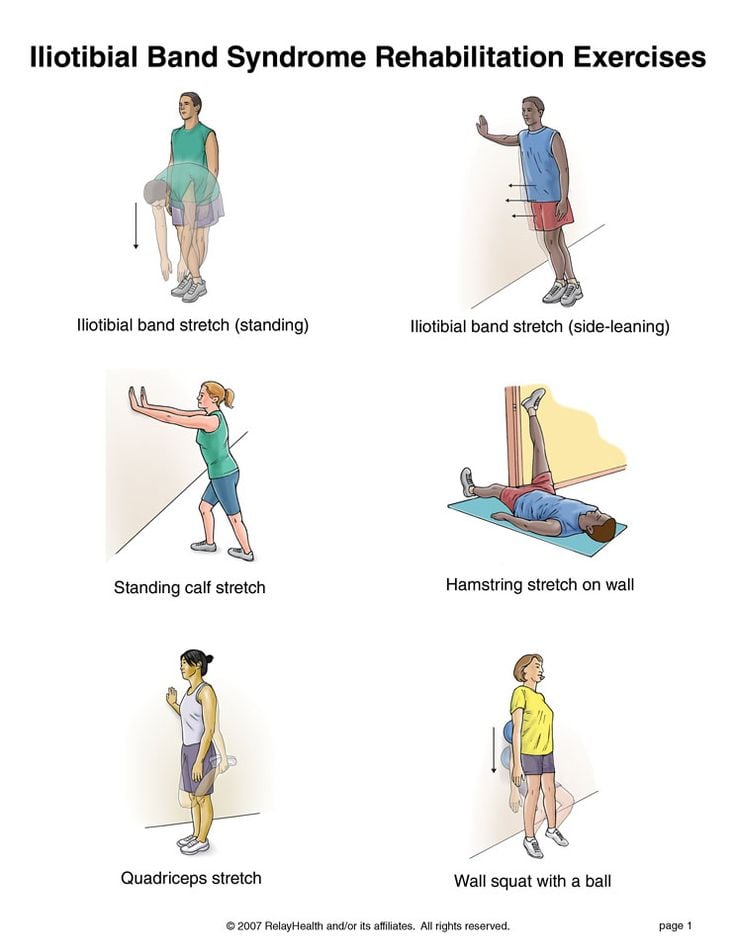
That sounds logical enough, but new research shows this is more myth than fact.
For one thing, people with tight iliotibial bands get knee pain just as often as people with normal iliotibial bands.
Basic anatomy also argues against this idea. The iliotibial band doesn’t rub directly against the edge of the tibia. It may feel and look that way on anatomy charts, but, as researchers concluded in a 2007 study, “. . . the perception of movement of the ITB across the epicondyle is an illusion.”
Another kink in the idea of stretching your iliotibial band to relieve knee pain is, well, you can’t stretch it. There are several reasons for this:
- Due to the position and attachment points of the iliotibial band, the most common stretches for the iliotibial band aren’t able to pull on it to any meaningful degree.
- The iliotibial band is anchored to the entire length of the femur in multiple places, so even if you could get your body into a position where you could stretch it, it probably wouldn’t budge.
- The iliotibial band is relatively flexible already, and while it can stretch a little, it immediately snaps back to its original length.
If we look at the studies on stretching and pain in general, the results are even less impressive.
There’s very little evidence that stretching any joint reduces pain or soreness. Some research shows stretching might help reduce pain, but the effects are so small that they aren’t much different from doing nothing.
Another study found that active release technique (ART), a specific kind of stretching, helped reduce neck pain, but the improvements were miniscule.
That said, stretching could reduce inflammation in connective tissue, and inflammation could be one contributor to joint pain. Right now, though, no one knows for sure. If inflammation isn’t the cause of your knee pain, then it’s even less likely this would help.
So, what’s causing the pain then?
Well, it’s more likely that “iliotibial band” pain is actually caused by the compression and irritation of the fat and nerves underneath the iliotibial band. When this tissue is surgically removed, the pain goes away.
The bottom line is that knee pain isn’t caused by a tight iliotibial band, and stretching your iliotibial band isn’t going to fix your knee pain. Stretching may help reduce the perception of pain in the short term, but there’s no evidence becoming more flexible will help prevent or reduce knee pain in the long term.
Knee Pain and Squatting
Heavy, strenuous squats look like they must be bad for your knees, and many doctors are quick to tell you that if you have knee pain, you should stop squatting.
The general idea is that every rep of a heavy, deep squat puts a little more wear on the cartilage and tendons in your knees. Over time this contributes to knee pain and potentially disastrous injuries like a tendon rupture.
Scientists at Duke University debunked this myth in a study that examined two decades of published research on this question.
They found that during the squat . . .
The hamstrings stabilize the shinbone in such a way that stress on the knee joint isn’t harmful.
The actual forces placed on the connective tissue in the knee are well within the safe, acceptable range. In one study, the highest ACL force recorded when squatting was a mere 6 percent of its ultimate strength, and in another it was only 25 percent. The highest recorded PCL forces were well within natural strength limits as well.
Other research has shown that powerlifters, who squat deep and heavy, often have greater knee stability than other athletes, and experienced weightlifters have joints that are just as healthy as the average person. These people were also training with loads that put more than six times their body weight on the knee joint.
The bottom line is that as long as you squat with proper form, squats aren’t bad for your knees.
Knee Pain and Massage
Massage feels good, has very few risks, and is used by many people to reduce pain, but how well does it really work?
Research goes back and forth. Some studies show massage reduces joint pain and others don’t, but on the whole it looks like it’s better than doing nothing.
It’s also hard to say if the (small) benefits of massage therapy are due to the massage, or from a more general improvement in mood.
Massage reduces anxiety and depression, which are both linked with joint pain, so it’s possible that simply feeling better is what makes the pain diminish.
The bottom line is that massage may help reduce your knee pain and certainly won’t hurt, but it’s far from a sure bet. If you can afford it, it’s probably worth a shot.
Knee Pain and Chiropractic
Chiropractic is a form of alternative medicine based on fixing misaligned joints, especially the spine, by manually pushing and pulling them back into position. In theory, realigning joints this way improves the function of nerves, muscles, and other organs in the body.
No studies have directly measured how chiropractic affects knee pain, but the little evidence available doesn’t look good.
Most studies show chiropractic doesn’t reduce joint pain, and the few that do also show that it’s not any more effective than other kinds of therapy.
The few half-decent studies that show even a glimmer of hope also used other therapies for knee pain in addition to chiropractic, so there’s no way to know which treatment actually helped reduce pain. Given that most studies on chiropractic alone show that it doesn’t work, it’s more likely the other techniques were responsible for the improvements.
There isn’t even a plausible mechanism for how chiropractic could help reduce knee pain.
There are a handful of studies that people throw around as proof that chiropractic works, but upon closer scrutiny it’s clear they don’t prove anything of the sort.
For example, most of these studies only measure pain immediately before and after people get chiropractic, and it’s a well-known fact that people are more likely to experience a placebo effect during that period.
Studies on all forms of chiropractic are notorious for other flaws, such as . . .
- Poor blinding (which raises the chances of a placebo effect interfering with the results).
- Small samples size (which increases the chances of finding a false-positive result).
- Minimal or incomplete reporting of the results (which makes the results seem more impressive than they really are).
To be fair, many people say that chiropractic helps them feel better, and there’s truth to the idea that, “If it works, it works.” On the other hand, chances are good that any improvement is more likely a placebo effect, so don’t count on chiropractic to actually fix whatever is wrong with your knee.
The bottom line is that there’s little evidence that chiropractic will reduce knee pain, and if it does help you feel better, chances are good it was through a placebo effect.
Knee Pain and Foam Rolling
Foam rolling is a kind of self massage that involves using a foam tube to rub and compress muscles.
Depending on who you ask, one of the main arguments for foam rolling is the idea that pain is caused by trigger points—patches of connective tissue called fascia that get become overstimulated, tight, and painful. Fascia is a web of connective tissue beneath the skin that attaches, protects, and separates muscles and other internal organs.
(There are multiple definitions for trigger points, which is part of why the science surrounding them is so fuzzy, but that’s the generally agreed upon explanation).
In theory, kneading these trigger points with a foam roller, tennis ball, or a stick helps release these tight patches of fascia, thus reducing pain.
There are several parts of this theory that don’t add up, though:
- The parts of a muscle that feel the tightest and most painful are, objectively, often the softest parts of the muscle. That’s the opposite of what you’d expect if “tight” fascia were causing pain.
- Trigger point experts often can’t agree what the different trigger points are or how to find them, so it’s hard to say that foam rolling them is a reliable way to reduce pain.
- Studies on trigger point therapy are all over the place. Some show that it helps reduce pain and others don’t, and none of the results are impressive.
Foam rolling aficionados also generally say that you should target the iliotibial band, but, as you now know, “tight” iliotibial bands aren’t what causes knee pain.
All in all, the evidence for foam rolling is probably one rung down from getting a professional massage. It’s likely better than doing nothing, but not much.
The bottom line is that there’s almost no evidence that foam rolling reduces knee pain, but it’s probably better than nothing if it makes you feel better.
Knee Pain and Acupuncture
Acupuncture is a kind of alternative medicine that involves poking the skin or tissues with extremely thin needles to alleviate pain and to treat various physical, mental, and emotional problems.
Some people say acupuncture works because it “rebalances” the lifeforce of your body, called “qi.” Others say it works because it stimulates the body to produce more painkilling chemicals. And others don’t try to justify why it works.
What do studies show, though?
Well, it depends on where you look for answers.
It’s easy to find reviews and meta-analyses that seem to show acupuncture works, but it’s a different story when you look at these studies individually.
Review studies and meta-analyses on acupuncture often play a kind of statistical sleight of hand. The highest quality studies show insignificant effects, but a few low-quality studies show profound effects, so the researchers throw them all together and essentially “average out” the results, which lets them conclude that acupuncture works.
What makes some studies low-quality, you wonder?
Here are three of the most common scientific sins of acupuncture research:
- First, most of the studies are poorly blinded, which means it’s too obvious to either the researchers or the subjects who’s receiving the treatment (and this can skew the results in favor of acupuncture).
- Second, when you’re dealing with pain, providing just about any type of treatment is better than simply doing nothing (thanks to the placebo effect).
- Third, the few positive results are disappointingly small. For example, people who get acupuncture for knee pain typically say their pain improves by 4 points on a 20 point scale, and people who get a placebo treatment say their pain improves by 3 points on a 20 point scale. This is so small that it’s meaningless in the real world, but depending on how the study is designed, this can pass for statistically significant.
If you throw out the garbage research and only look at the best studies, you quickly find that acupuncture either doesn’t work or slightly reduces pain for a week or two and then stops working. Even then, the results are so small that they’re almost nonexistent in most cases.
The bottom line is that there’s very little evidence that acupuncture can reduce knee pain, and in most cases, it’s no better than doing nothing.
Knee Pain and Weight Loss

If joint pain is caused by excess wear and tear, then it makes sense that carrying around an extra 10, 20, or 30 pounds of body fat would be bad for your knees.
Sure enough, that seems to be the case.
Excess body weight is generally associated with more knee pain in athletes and sedentary people and for the young and old alike.
Specifically, overweight men and women are four to five times more likely to develop osteoarthritis, which is the gradual degeneration of cartilage in joints. Osteoarthritis is different from rheumatoid arthritis, but both involve increased levels of inflammation and cartilage degeneration.
Due to the mechanics of the knee joint, every pound of weight loss translates into about four pounds of reduced load on the knee, which is why reaching a healthier weight (going from obese to overweight or overweight to normal weight) reduces your chances of developing knee joint degeneration by 20 to 30 percent.
In other words, losing 20 pounds is the equivalent of losing 80 pounds as far as your knees are concerned.
But there’s more to the story.
Obese people have higher rates of joint degeneration in their wrists, fingers, and shoulders.
Why?
Shouldn’t being overweight just hurt load-bearing joints like the hips, knees, and ankles? Why would it damage other joints, too?
Well, the answer seems to be that obesity damages joints partly by raising levels of inflammation in the body. Knee joint degeneration is also linked with higher levels of inflammation, which further explains why losing weight protects your knees.
The good news is that it only takes about a 10 percent loss of body weight to significantly reduce whole-body inflammation, which could significantly reduce or eliminate damage to the knee.
The bottom line is that maintaining a healthy weight is one of the best things you can do to reduce and prevent knee pain and joint damage. If you’re currently overweight and have knee pain, losing weight should be your number one priority.
Knee Pain and Posture
Poor posture just looks . . . unhealthy.
Surely, hunching over like some gollum wannabe must be bad for your shoulders, back, and knees, right?
Poor posture is also immediately recognizable, easy to fix, and thus, a tempting scapegoat for all kinds of aches and pains.
This is why movement gurus everywhere say that small quirks in your posture, like putting more weight on one leg when you stand, gradually pull your body out of alignment. This forces other parts of your body compensate by altering their movement, which leads to knee pain over time.
If you fix your posture, they say, then everything will fall back into alignment and the pain will go away.
*Sigh* If only it were that easy . . .
It turns out that all of this is more or less hogwash.
There’s very little evidence that small irregularities in posture, movement, or the alignment of your joints increase your risk of any kind of joint pain.
This idea has been thoroughly debunked for knee pain, back pain, and many other kinds of joint pain.
One of the main nails in the coffin for this idea is evidence that people experience pain with no signs of physical injury or “misalignment,” and there are other cases where people have serious structural damage like dislocated vertebrae, but no pain.
Other studies have shown that muscle imbalances and variations in posture also aren’t linked with joint pain.
This isn’t to say that poor posture couldn’t have any effect on knee pain, but it’s rarely the main cause. Now, there are obviously other reasons to improve your posture, but avoiding knee pain shouldn’t be one of them.
The bottom line is that poor posture is almost certainly not the main cause of your knee pain.
Knee Pain and NSAIDs

Non-steroidal anti-inflammatories (NSAIDs) are a class of drugs that blocks chemicals made by your body that increase pain, swelling, and inflammation.
Some of the most common NSAIDs are ibuprofen (Advil), naproxen (Aleve), and celecoxib (Celebrex).
There are two main reasons people take NSAIDs for joint pain:
- To reduce pain in the short term.
- To reduce inflammation, which many think is the cause of joint pain.
In the short term, NSAIDs can reduce pain, which is why they aren’t a bad choice if you’re only taking them for a few days to get through the worst of the pain.
If your knee pain is caused by inflammation, then NSAIDs may also be able to help fix the actual cause of your pain, and not just reduce pain.
Unfortunately, many knee injuries aren’t inflamed, which means painkillers like NSAIDs aren’t actually healing your knee. This is why most NSAIDs don’t work well for reducing joint pain for more than a few days or weeks.
So, if it just makes your knee feel better, what’s the problem with taking them?
Well, there are a few risks with NSAIDs, too.
First, gastrointestinal problems like ulcers have been noted with long-term NSAID use. This doesn’t happen often, but it’s possible.
Second, it’s possible to mask knee pain with NSAIDs and thereby make it easier to keep training, which can delay healing even further. In other words, if you hide the pain with NSAIDs, it’s easier to re-injure your knee by training harder than you otherwise would.
That said, assuming you’re otherwise healthy, there’s no reason you can’t take NSAIDs for a few days to get through the worst of the pain if you injure your knee.
The bottom line is that NSAIDs can reduce pain for a few days or weeks, but they don’t work well for healing knee injuries or reducing pain long term. If you take them to cover up knee pain so you can keep training, chances are good you’ll only re-injure your knee.
Knee Pain and Glucosamine Chondroitin
Glucosamine and chondroitin are structural components of collagen, the main protein that forms cartilage.
Both compounds are produced naturally by the body, but they’re also sold together as the supplement glucosamine-chondroitin. The idea is that by providing the body with more of these two chemicals, you can improve joint health.
It hasn’t panned out that way, though.
This was proven in a massive double-blind, randomized controlled trial on 1,583 people with knee pain that was published in the New England Journal of Medicine. The researchers gave some people glucosamine, some chondroitin, some both glucosamine and chondroitin, some NSAIDs, and the final group a placebo.
After two years, there was no difference in knee pain between the group that took glucosamine chondroitin (together or individually) and the people who took the placebo.
Additionally, studies have repeatedly shown that glucosamine chondroitin isn’t effective for reducing joint pain or improving cartilage health.
There’s no evidence that joint pain is caused by a lack of glucosamine and chondroitin, so it doesn’t make sense that supplementing with these compounds would reduce joint pain.
It flat out doesn’t work.
The bottom line is that glucosamine chondroitin supplements have never been proven to reduce or prevent knee pain.
Knee Pain and Icing
The idea behind icing goes like this:
- Inflammation causes pain and makes it harder for injuries to heal.
- Reducing inflammation will reduce pain and help injuries heal faster.
- Icing reduces inflammation.
- Therefore, icing reduces pain and helps you heal faster.
This logic has made icing standard dogma for decades—if any joint hurts, you should ice it early and often.
Recently, though, the pendulum has swung in the other direction. Now, experts warn that icing can actually slow healing and prolong joint pain.
The good news is that both groups are wrong.
There’s very little evidence that icing helps, hurts, or does anything to your joints.
The same thing is true of alternating between icing and warming, known as “contrast therapy,” it doesn’t seem to do much of anything.
That said, icing can take the edge off of pain and reduce your need for NSAIDs, but it’s not going to make knee pain go away faster over the long term.
The bottom line is that icing has never been proven to reduce joint pain, but it can temporarily reduce your knee pain by numbing the area.
Knee Pain and Physical Therapy

Physical therapy, also called physiotherapy (PT), involves using exercises, special devices, and education to help people regain or preserve healthy movement.
PT can involve any number of different treatments from massage to special movement exercises to medical devices that reinforce proper movement. Different physical therapists also have different methods and recommend different techniques, so it’s hard to say across the board whether it “works” or not.
On the whole, physical therapy seems to help reduce knee pain.
The effects aren’t huge, and it doesn’t work all of the time or equally well for everyone, but by and large it’s better than doing nothing.
One of the most well-supported forms of physical therapy for repetitive strain injuries is to gradually stress the weakened structures in the knee joint with progressive exercise, which causes them to grow stronger and heal.
For example, using leg extensions to build up the connective tissues in your patellar tendon.
Interestingly, one thing that’s clear is the people who are happiest with their physical therapist generally have the best results. Whether that’s because simply feeling like you’re in the hands of a trained, kind professional reduces pain, or whether these people liked their therapist more because they did a great job, isn’t clear.
What we can say, is that if you decide to see a physical therapist, make sure it’s someone you like.
The bottom line is that physical therapy might help reduce knee pain, but that depends on what’s causing the pain and what the therapist recommends.
Knee Pain and Prolotherapy
Prolotherapy, or “proliferation therapy,” involves injecting an irritant into a tendon, muscle, or joint to promote the growth of new tissue.
Typically, either a sugar solution (dextrose) or a purified form of cod liver oil (sodium morrhuate) is injected every few weeks for several months. The idea is that by irritating the surrounding tissue, you can encourage the body to heal itself.
Researchers have tested prolotherapy on all kinds of muscle and joint pain, including . . .
. . . and the best we can really say is that it might help reduce pain for some problems, but most of the time it either doesn’t work or the benefits are so small it’s impossible to tell.
The underlying mechanism for why prolotherapy might work has also never been proven, and studies show that there’s no increase in cartilage growth after prolotherapy injections.
The bottom line is that prolotherapy probably doesn’t reduce knee pain, and almost certainly isn’t worth the cost, inconvenience, and discomfort of having to get repeated injections.
Knee Pain and Transcutaneous Electrical Nerve Stimulation (TENS)
Transcutaneous Electrical Nerve Stimulation (TENS) involves using a device to send an electric current through the skin to stimulate nerves and reduce pain.
Sending an electric current through the skin can cause some odd sensations and muscle contractions that could “drown out” pain, and it may be able to suppress pain signals in the brain, but that doesn’t necessarily fix the underlying problem.
One review study on TENS found that it helps about half the time and doesn’t help the other half. Other studies are even less positive, and show it probably just doesn’t work for joint pain (although it might help other conditions, like nerve damage caused by diabetes).
The bottom line is that TENS might help reduce some kinds of pain, but it probably won’t work for knee pain.
Knee Pain and Corticosteroid Injections
Cortisone is a kind of steroid that reduces inflammation. A corticosteroid injection, or cortisone shot, is an injection of cortisone into a tendon to reduce inflammation and pain.
They’re often used for joint pain such as carpal tunnel syndrome, knee pain, and low-back pain.
Cortisone shots can reduce inflammation and knee pain in the short term, but as soon as the drugs start to wear off, the pain returns.
A recent review conducted by researchers at the University of Bern in Switzerland analyzed 27 studies on cortisone shots for knee pain. The result?
Cortisone shots sometimes reduce knee pain for a few weeks, but the effects are small, unreliable, and short-lived.
Steroid injections also have risks.
Some researchers also think there’s a link between cortisone shots and tendon damage, and other studies have shown that people who get cortisone shots heal slower than people who simply rest.
The link between cortisone shots and joint damage isn’t airtight, but it’s not comforting, either.
The bottom line is that, in most cases, cortisone shots aren’t going to reduce your knee pain for long, won’t do anything to heal your knee, and usually aren’t worth the cost, inconvenience, and risk.
Knee Pain and Curcumin

Curcumin is a yellow pigment found in the turmeric plant, which is the main spice in curry.
It’s been used therapeutically in Ayurvedic (Indian) medicine for thousands of years, but recently it’s been getting more and more attention in the scientific community as well.
Scientific researchers around the world are studying its ability to fight a variety of disease such as cancer, cardiovascular disease, osteoporosis, diabetes, Alzheimer’s, and more.
The main benefit seems to be curcumin’s powerful anti-inflammatory effects. Curcumin supplementation inhibits proteins that trigger the production of inflammatory chemicals, and research shows it may be as effective for reducing knee pain as ibuprofen.
Curcumin has a significant downside, however: intestinal absorption is very poor. So much so that supplementation without enhancement more or less eliminates the majority of its health benefits.
Fortunately, there’s an easy solution for increasing bioavailability—black pepper extract. Research shows that pairing black pepper extract with curcumin increases bioavailability twentyfold. And when you do that, curcumin becomes an effective joint support supplement.
The bottom line is that curcumin may help reduce knee pain, potentially as much as ibuprofen, but you need to take it with black pepper extract for it to be effective.
Knee Pain and Rest
Some people say that as soon as your knee starts hurting, you should stop working out completely and rest as long as you need to before you do any kind of exercise.
There’s some truth to that—most people have a tendency to “push through the pain,” which only makes the problem worse.
But you don’t want to stop working out entirely.
In general, complete rest actually increases pain or delays healing compared to light activity. Other research on both repetitive strain injuries and traumatic injuries shows that light exercise helps connective tissue heal faster.
So, while you don’t want to keep doing any activities that cause pain, you want to stay as active as you can without causing your knee to hurt any more than it already does.
I saved this for last because, right now, active rest is about the most well-supported treatment for knee pain out there. If moving your knee in a particular way hurts, then stop moving your knee that way until it stops hurting.
The bottom line is that active rest—moving your knee as much as possible without experiencing any pain—is the most reliable way to reduce knee pain.
7 Ways to Reduce and Prevent Knee Pain
At this point you’re probably thinking, “Great, so what the hell am I supposed to do about my knee?”
Well, that’s what you’re about to learn.
There are seven things you can do that will reduce knee pain in most cases. None of them are guaranteed fixes, but they’re your best options.
The first technique is by far the most reliable. After that, the remaining six fall into the category of “throw it at the wall and see what sticks.” They might help, but they’re also unlikely to hurt, so there’s no harm in trying them.
Knee Pain Solution #1
Stop Doing Whatever Makes Your Knee Hurt
If your knee hurts during certain exercises, and you haven’t been through some traumatic injury, then chances are good you’re dealing with some kind of repetitive strain injury (RSI).
To understand why, we need to look at what happens to your body when you exercise in the first place.
When you lift weights, the tissues in your muscles, tendons, and joints sustain small amounts of damage. Between workouts, your body repairs as much of the wear and tear as it can and, provided you allow enough time for recovery, these tissues get stronger and more durable over time.
Sometimes, though, this wear and tear builds up faster than your body can repair it, and things start hurting.
As mentioned earlier, the single biggest mistake people make when dealing with repetitive stress injuries is they ignore the early warning signs and keep training as normal. Sometimes the pain goes away on its own, but most of the time, you’re just digging yourself into a deeper and deeper hole.
This is how a minor, niggling pain can grow into a debilitating injury that takes months to heal.
Luckily, the solution is simple—rest.
Assuming you just have an RSI, and you’re otherwise healthy, your body shouldn’t have any trouble repairing itself.
Now, the annoying part is that some injuries can take a while to heal, which means taking weeks or even months away from the activity that caused the injury.
Tendon injuries are one of the most frustrating, as they typically take much longer to heal than other kinds of damage.
The good news is that you don’t have to stop exercising altogether. Studies show that active rest, doing light activity but avoiding anything that causes severe pain, can help you heal faster.
So, as a general rule, the best way to reduce knee pain is to move your knee as much as possible without experiencing pain.
There are two approaches you can take to this:
- Immediately stop lifting weights and start doing other activities, like walking, that don’t irritate your knee.
- Modify your lifting plan to work around your knee pain.
Both approaches have pros and cons.
If you take the first option, then there’s almost zero chance of prolonging your knee pain, but you also have to stop doing any kind of weightlifting.
If your knee’s been hurting for a while or the pain is intense, then this is a better option. The easiest way to practice active rest is to pick a different form of exercise, like walking, cycling, rowing, hiking, or swimming, and start doing that for at least 30 minutes a day.
If you take the second option, then it might take longer to heal, but you also get to keep going to the gym.
If your knee doesn’t hurt much, hasn’t been hurting for long, or only hurts when you do certain exercises, this might be the better option.
Let’s say your knee hurts when you squat. Here’s how you might go about modifying your plan:
- Use different variations of squats that don’t hurt, such as front squats, high-bar squats, pause squats, or split squats.
- Stop doing all squat-type exercises.
- Stop doing all lower body exercises.
- Stop lifting until you feel better.
One thing to know before we move on: some people will tell you that if you feel any pain while working out, then you should stop training.
That’s a safe bet, but it’s also true that you can still have knee pain long after the actual damage has healed.
Ultimately, when you start lifting again is a judgement call you’ll have to make on your own, but here’s a good rule of thumb:
If the pain is intense, constant, and gets worse during certain lifts, then you need to give yourself more time to heal before you start training again.
If the pain is mild, intermittent, and doesn’t seem to get worse during certain exercises, then you can probably start training again without having to worry that you’ll prolong the pain.
Knee Pain Solution #2
Improve Your Knee Mobility

Mobility refers to how well you can move a joint through its natural range of motion.
When it comes to the knee, this means being able to flex and extend your lower leg without feelings of tightness when doing exercises like the squat, lunge, and deadlift.
As we covered earlier, there isn’t much evidence that stretching prevents or reduces knee pain, but it’s also not going to hurt, and many people find it helps them feel better in the short term.
It’s also possible that if you don’t have the mobility to do lower body exercises properly, then you could be setting yourself up for an overuse injury (theoretically, at least).
Most knee mobility exercises involve using simple stretches or tools like foam rollers, elastic bands, and lacrosse balls to massage and stretch the muscles around your quadriceps, hamstrings, and iliotibial band.
If you want to learn more about how to increase your knee mobility, then check out this article:
Knee Pain Solution #3
Increase Your Knee Strength
If you aren’t currently lifting weights, and doing so doesn’t hurt your knee, then you should start.
Increasing leg strength is one of the more reliable ways to avoid knee pain, and the same thing is true of other kinds of pain as well.
You need to be careful, though, because if you’re already dealing with knee pain then more exercise can also make the problem worse.
As you probably know, it’s often hard to tell how hard you should train or how many sets and reps you should do without causing further damage.
This is why it pays to keep track of your knee pain and adjust your training accordingly. Here’s how:
1. Pick an exercise that you can do to easily test your level of knee pain. A common method that’s used in research is to do a single-leg squat with your heel elevated or on a decline surface, like this:
2. Rate your level of pain on a scale of 1 to 10. If the number is a three or less, then go ahead with your workout. If it’s higher than that, stick to exercises that don’t bother your knee or skip lifting and do a different activity that day.
3. Do the same test every day, at the same time, and track your level of pain. If it gets worse over time, then you need to dial back on your workouts and rest your knee more. If the pain is the same or less, then you can keep training as much as you are now or do even more.
If you’d like to learn how to increase your leg strength, check out this article:
The Ultimate Leg Workout: The Best Leg Exercises for Big Wheels
Knee Pain Solution #4
Use Proper Form In Your Weightlifting
Weightlifting injuries are less common than most people think, but when they do happen, it’s often because the person wasn’t using proper technique.
Form mistakes go far beyond the heavy half repping that gives a bad name to the big compound lifts like the squat, deadlift, bench press, and military press. You can work with proper amounts of weight and use a full range of motion and still put yourself at a considerable risk of injury.
For instance…
- If you let your knees bow in when you squat, or extend them too far past your toes, you can really hurt them when going heavy.
- If you round your back during a deadlift, or hyperextend it too far at the top, you’re asking for a lower-back injury.
- If you flatten your back and round your shoulders at the top of a bench press, or flare your elbows out too much, you will probably have shoulder and elbow problems at some point.
Most exercises have little quirks like these, which is why you should take the time to learn proper form on everything you’re doing, and make sure to stick to it.
Bodybuilding.com’s videos are a great resource for this, and you may also like the following articles on how to do some of the most important lifts:
The Deadlift and Your Lower Back: Harmful or Helpful?
Squatting and Your Knees and Back: Injury Risk or Safe?
The Ultimate Guide to the Military Press: The Key to Great Shoulders
Knee Pain Solution #5
Warm Up Properly
Many people’s warm-up routines consist of a few minutes of static stretching.
This is a bad way to go about it.
Static stretching before exercise has been shown to impair speed and strength, and not only fail to help prevent injury, but possibly increase risk of injury due to the cellular damage it causes to muscle and its analgesic effect.
A proper warm-up routine should bring blood to the muscles that are about to be trained, increase suppleness, raise body temperature, and enhance free, coordinated movement.
The best way to do this is to move the muscles repeatedly through the expected ranges of motion, which does reduce the risk of injury.
That’s why it’s best to stick to a simple, short, multi-set warm-up routine like the one you’ll find in the books Bigger Leaner Stronger and Thinner Leaner Stronger, that goes like this:
First Warm-Up Set
8 reps with 50% of your working set weight
Rest 1 minute
Second Warm-Up Set
6 reps with 50% of your working set weight
Rest 1 minute
Third Warm-Up Set
4 reps with 70% of your working set weight
Rest 1 minute
Fourth Warm-Up Set
1 rep with 90% of your working set weight
Rest 2 minutes and then start your workout
By doing this warm-up routine, you’ll probably find that you can lift more weight while maintaining proper form, which can significantly reduce your risk of injury.
Many people also like to use knee sleeves to keep their joints warm during lower body workouts. They won’t reduce your risk of knee injury, but they aren’t going to hurt, either.
Both SBD and Rehband make good ones, if you want to give them a shot.
Knee Pain Solution #6
Massage Your Knee
Massage is one of the safest, least invasive things you can do to reduce knee pain.
There isn’t much evidence for or against it, but many people find it helps reduce pain at least for a while.
It might help, and probably won’t hurt, so it’s worth trying if you can afford it.
Knee Pain Solution #7
Take the Right Supplements
Compared to active rest and following a proper workout routine, supplements are going to have a very, very small impact on how fast your knee pain goes away.
Supplements don’t heal injuries. Training properly, eating a healthy diet, and giving yourself enough (but not too much) rest, does.
Some of the most popular supplements for joint pain, like glucosamine chondroitin, have also been thoroughly debunked.
That said, there are safe, natural substances that science indicates may help prevent and reduce knee pain.
(And if you’d like to know exactly what supplements to take to keep you healthy, injury-free, and full of vitality take the Legion Supplement Finder Quiz.)
Let’s quickly review the supplements that are most likely to help.
Fish Oil
Fish oil is known for being anti-inflammatory, and in cases where knee pain is caused by inflammation, taking fish oil may help.
The two main ingredients in fish oil, eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), improve the production of anti-inflammatory compounds in the body.
If you eat several servings of fatty fish like salmon, mackerel, sardines, and cod every week, you may not benefit from supplementation with fish oil. If you don’t, however, it’s a good idea to include it in your daily supplement regimen.
And if you’re looking for a high-quality fish oil, then you want to check out Triton.
It’s a high-potency, 100% triglyceride fish oil with added vitamin E to prevent oxidation and rancidity, and natural lemon oil, which prevents noxious “fish oil burps.”
Furthermore, it’s made from sustainably fished deep-water anchovies and sardines and is molecularly distilled to remove synthetic and natural toxins and contaminants.
So, if you want to optimize your mental and physical health and performance and reduce the risk of disease and dysfunction, like knee pain, then you want to try Triton today.
Curcumin
Studies show that supplementation with curcumin and black pepper extract reduces inflammatory signals in the joints and, in those with arthritis, relieves pain and stiffness and improves mobility.
When paired with piperine, the clinically effective dosages of curcumin range between 200 and 500 milligrams.
And that’s why there’s 500 mg of curcumin and 25 mg of piperine in each serving of our joint supplement, FORTIFY.
FORTIFY contains a clinically effective dose of curcumin in every serving along with three other ingredients also proven to enhance joint health and function:
- Undenatured type ll collagen
- Boswellia serrata
- Grape seed extract
The bottom line is if you want healthy, functional, and pain-free knees that can withstand the demands of your active lifestyle, then you want to try FORTIFY today.
Undenatured Type ll Collagen
Collagen is the main component of your body’s connective tissues, which means it serves as the primary building block for various things in it, including your skin, teeth, cartilage, bones, and tendons.
The collagen found in supplements comes from the connective tissue in animals, such as cows, chickens, and fish, and while there are over 37 different kinds of collagen in animals, they can be divided into two main categories:
- Type I collagen is the most abundant collagen of the human body, and is present in scar tissue, tendons, ligaments, skin, bones, and more.
- Type II collagen is the collagen that preserves joint function and protects them against damage.
In some cases, your body’s immune system can begin tearing down your own cartilage, in a condition known as arthritis.
Studies show that type II collagen can help alleviate this condition by “teaching” the immune system to stop attacking the proteins in joint cartilage, which in turn can significantly improve joint health and function and decrease or even eliminate pain and swelling.
In other words, type II collagen supplements can work like a natural vaccine of sorts, allowing your body to recognize its own joint collagen as a safe substance, thereby switching off the autoimmune response.
And the best part about type II collagen supplements is that these effects have been demonstrated in people with arthritic conditions and people with healthy joints.
The clinically effective dose of collagen is between 10 to 40 milligrams per day for improving joint health.
That’s a rather large range for dosing, but that’s only because studies have shown benefits using various doses, and it isn’t clear if more is better. Research clearly shows that 10 milligrams is effective, but not that two, three, or four times that amount is necessarily better.
This is why Fortify contains a clinically effective dosage of 10 milligrams of undenatured type ll collagen in every serving.
Pycnogenol
Pycnogenol is another compound derived from the bark of the maritime pine tree, or Pinus maritima.
It’s similar to white willow bark in that it works by reducing the production of inflammatory compounds in the body, and it also seems to reliably reduce joint pain.
The clinically effective dosage of pycnogenol is 100 to 200 mg per day.
The downside of pycnogenol is that it’s also expensive, which is why most supplements use a similar compound known as grape seed extract. Both of these compounds contain what are known as procyanidins, which are chains of antioxidants found in some plants. Although they aren’t exactly the same, it’s likely that grape seed extract offers many of the same benefits.
The clinically effective dosage of grapeseed extract is 75 to 300 mg per day, which is why Fortify contains 90 mg of grape seed extract per serving.
Boswellia Serrata
Boswellia serrata is a plant that produces an aromatic substance known as frankinsence, which has been used for thousands of years in Ayurvedic medicine to treat various disorders related to inflammation.
Thanks to modern science, we now know why.
Frankinsence contains molecules known as boswellic acids. Research shows that, like curcumin, boswellic acids—and one in particular known as acetyl-keto-beta-boswellic acid, or AKBA—inhibit the production of several proteins that cause inflammation in the body.
And in case you’re wondering, the difference between the anti-inflammatory mechanisms of curcumin and boswellic acids is they work on different enzymes. Curcumin inhibits an enzyme known as cyclooxygenase, or COX, and boswellic acids inhibit lysyl oxidase, or LOX (and, most notably, 5-LOX).
These anti-inflammatory properties extend to the joints, which is why studies show that Boswellia serrata is an effective treatment for reducing joint inflammation and pain as well as inhibiting the autoimmune response that eats away at joint cartilage and eventually causes arthritis.
The clinically effective dosages of Boswellia serrata range between 100 and 200 milligrams.
This is why there is 150 mg of Boswellia serrata in each serving of Fortify.
White Willow Bark
White willow bark is similar to aspirin (which is a synthetic version of a chemical that’s also found in willow), that’s been used to reduce pain and inflammation for thousands of years.
It works by blocking the production of inflammatory compounds produced in the body, and it works about as well as other NSAIDs.
The clinically effective dosage of white willow bark is 240 milligrams per day.
Oh, and if you aren’t sure if the supplements discussed in this article are right for your budget, circumstances, and goals, then take the Legion Supplement Finder Quiz! In less than a minute, it’ll tell you exactly what supplements are right for you. Click here to check it out.
The Bottom Line on Knee Pain
Knee pain is one of the most common hurdles for us fitness folk.
Unfortunately, most of the things that “everyone knows” help reduce knee pain either don’t have any evidence for them or have been debunked.
While it’s impossible to know what causes knee pain in every instance, one of the most common culprits is a repetitive strain injury, or RSI. These can take anywhere from weeks to months to heal, but you can speed up the process by sticking to the following seven steps:
- Stop doing whatever makes your knee hurt.
- Improve your knee mobility.
- Increase your knee strength.
- Use proper form in your weightlifting.
- Warm up properly.
- Massage your knee.
- Take the right supplements.
Do that, and chances are good you’ll be back in the gym in a few weeks.
What’s your take on knee pain? Have anything else to share? Let me know in the comments below!
Scientific References +
- Bost, J., Maroon, A., & Maroon, J. (2010). Natural anti-inflammatory agents for pain relief. Surgical Neurology International, 1(1), 80. https://doi.org/10.4103/2152-7806.73804
- Herman, K., Barton, C., Malliaras, P., & Morrissey, D. (2012). The effectiveness of neuromuscular warm-up strategies, that require no additional equipment, for preventing lower limb injuries during sports participation: a systematic review. BMC Medicine, 10. https://doi.org/10.1186/1741-7015-10-75
- McMillian, D. J., Moore, J. H., Hatler, B. S., & Taylor, D. C. (2006). Dynamic vs. static-stretching warm up: The effect on power and agility performance. Journal of Strength and Conditioning Research, 20(3), 492–499. https://doi.org/10.1519/18205.1
- M A Moore, & R S Hutton. (n.d.). Electromyographic investigation of muscle stretching techniques - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/7453508/
- Macpherson, P. C. D., Schork, M. A., & Faulkner, J. A. (1996). Contraction-induced injury to single fiber segments from fast and slow muscles of rats by single stretches. American Journal of Physiology - Cell Physiology, 271(5 40-5). https://doi.org/10.1152/ajpcell.1996.271.5.c1438
- Hart, L. (2005). Effect of stretching on sport injury risk: A review. In Clinical Journal of Sport Medicine (Vol. 15, Issue 2, p. 113). Lippincott Williams and Wilkins. https://doi.org/10.1097/01.jsm.0000151869.98555.67
- La Torre, A., Castagna, C., Gervasoni, E., Cè, E., Rampichini, S., Ferrarin, M., & Merati, G. (2010). Acute effects of static stretching on squat jump performance at different knee starting angles. Journal of Strength and Conditioning Research, 24(3), 687–694. https://doi.org/10.1519/JSC.0b013e3181c7b443
- Winchester, J. B., Nelson, A. G., Landin, D., Young, M. A., & Schexnayder, I. C. (2008). Static stretching impairs sprint performance in collegiate track and field athletes. Journal of Strength and Conditioning Research, 22(1), 13–18. https://doi.org/10.1519/jsc.0b013e31815ef202
- Andersen, L. L., Kjær, M., Søgaard, K., Hansen, L., Kryger, A. I., & Sjøgaard, G. (2008). Effect of two contrasting types of physical exercise on chronic neck muscle pain. Arthritis Care and Research, 59(1), 84–91. https://doi.org/10.1002/art.23256
- Puett, D. W., & Griffin, M. R. (1994). Published trials of nonmedicinal and noninvasive therapies for hip and knee osteoarthritis. Annals of Internal Medicine, 121(2), 133–140. https://doi.org/10.7326/0003-4819-121-2-199407150-00010
- Khan, K. M., Cook, J. L., Bonar, F., Harcourt, P., & Åstrom, M. (1999). Histopathology of common tendinopathies: Update and implications for clinical management. Sports Medicine, 27(6), 393–408. https://doi.org/10.2165/00007256-199927060-00004
- Cook, J. L., Rio, E., Purdam, C. R., & Docking, S. I. (2016). Revisiting the continuum model of tendon pathology: What is its merit in clinical practice and research? In British Journal of Sports Medicine (Vol. 50, Issue 19, pp. 1187–1191). BMJ Publishing Group. https://doi.org/10.1136/bjsports-2015-095422
- Khan, K. M., Cook, J. L., Taunton, J. E., & Bonar, F. (2000). Overuse tendinosis, not tendinitis. Part 1: A new paradigm for a difficult clinical problem. In Physician and Sportsmedicine (Vol. 28, Issue 5, pp. 38–48). McGraw-Hill Companies. https://doi.org/10.3810/psm.2000.05.890
- Magnusson, S. P., Langberg, H., & Kjaer, M. (2010). The pathogenesis of tendinopathy: Balancing the response to loading. In Nature Reviews Rheumatology (Vol. 6, Issue 5, pp. 262–268). Nat Rev Rheumatol. https://doi.org/10.1038/nrrheum.2010.43
- Kjær, M., & Magnusson, S. P. (2008). Mechanical adaptation and tissue remodeling. In Collagen: Structure and Mechanics (pp. 249–267). Springer US. https://doi.org/10.1007/978-0-387-73906-9_9
- Mealy, K., Brennan, H., & C Fenelon, G. C. (1986). Early mobilisation of acute whiplash injuries. British Medical Journal (Clinical Research Ed.), 292(6521), 656–657. https://doi.org/10.1136/bmj.292.6521.656
- Helliwell, P. S., & Taylor, W. J. (2004). Repetitive strain injury. In Postgraduate Medical Journal (Vol. 80, Issue 946, pp. 438–443). The Fellowship of Postgraduate Medicine. https://doi.org/10.1136/pgmj.2003.012591
- Sorrenti, S. J. (2006). Achilles tendon rupture: Effect of early mobilization in rehabilitation after surgical repair. Foot and Ankle International, 27(6), 407–410. https://doi.org/10.1177/107110070602700603
- Hagen, K. B., Jamtvedt, G., Hilde, G., & Winnem, M. F. (2005). The updated cochrane review of bed rest for low back pain and sciatica. In Spine (Vol. 30, Issue 5, pp. 542–546). Spine (Phila Pa 1976). https://doi.org/10.1097/01.brs.0000154625.02586.95
- Shoba, G., Joy, D., Joseph, T., Majeed, M., Rajendran, R., & Srinivas, P. S. S. R. (1998). Influence of piperine on the pharmacokinetics of curcumin in animals and human volunteers. Planta Medica, 64(4), 353–356. https://doi.org/10.1055/s-2006-957450
- Giuseppe Garcea, David P Berry, Donald J L Jones, Raj Singh, Ashley R Dennison, Peter B Farmer, Ricky A Sharma, William P Steward, & Andreas J Gescher. (n.d.). Consumption of the putative chemopreventive agent curcumin by cancer patients: assessment of curcumin levels in the colorectum and their pharmacodynamic consequences - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/15668484/
- Anand, P., Kunnumakkara, A. B., Newman, R. A., & Aggarwal, B. B. (2007). Bioavailability of curcumin: Problems and promises. In Molecular Pharmaceutics (Vol. 4, Issue 6, pp. 807–818). Mol Pharm. https://doi.org/10.1021/mp700113r
- Kuptniratsaikul, V., Thanakhumtorn, S., Chinswangwatanakul, P., Wattanamongkonsil, L., & Thamlikitkul, V. (2009). Efficacy and safety of Curcuma domestica extracts in patients with knee osteoarthritis. Journal of Alternative and Complementary Medicine, 15(8), 891–897. https://doi.org/10.1089/acm.2008.0186
- Panahi, Y., Rahimnia, A. R., Sharafi, M., Alishiri, G., Saburi, A., & Sahebkar, A. (2014). Curcuminoid treatment for knee osteoarthritis: A randomized double-blind placebo-controlled trial. Phytotherapy Research, 28(11), 1625–1631. https://doi.org/10.1002/ptr.5174
- Aggarwal, S., Ichikawa, H., Takada, Y., Sandur, S. K., Shishodia, S., & Aggarwal, B. B. (2006). Curcumin (diferuloylmethane) down-regulates expression of cell proliferation and antiapoptotic and metastatic gene products through suppression of IκBα kinase and Akt activation. Molecular Pharmacology, 69(1), 195–206. https://doi.org/10.1124/mol.105.017400
- Coombes, B. K., Bisset, L., & Vicenzino, B. (2010). Efficacy and safety of corticosteroid injections and other injections for management of tendinopathy: A systematic review of randomised controlled trials. The Lancet, 376(9754), 1751–1767. https://doi.org/10.1016/S0140-6736(10)61160-9
- Fisher, P. (2004). Role of Steroids in Tendon Rupture or Disintegration Known for Decades [3]. In Archives of Internal Medicine (Vol. 164, Issue 6, p. 678). American Medical Association. https://doi.org/10.1001/archinte.164.6.678-a
- Jüni, P., Hari, R., Rutjes, A. W. S., Fischer, R., Silletta, M. G., Reichenbach, S., & da Costa, B. R. (2015). Intra-articular corticosteroid for knee osteoarthritis. In Cochrane Database of Systematic Reviews (Vol. 2015, Issue 10). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD005328.pub3
- Mohamadi, A., Chan, J. J., Claessen, F. M. A. P., Ring, D., & Chen, N. C. (2017). Corticosteroid Injections Give Small and Transient Pain Relief in Rotator Cuff Tendinosis: A Meta-analysis. In Clinical Orthopaedics and Related Research (Vol. 475, Issue 1, pp. 232–243). Springer New York LLC. https://doi.org/10.1007/s11999-016-5002-1
- DeSantana, J. M., Walsh, D. M., Vance, C., Rakel, B. A., & Sluka, K. A. (2008). Effectiveness of transcutaneous electrical nerve stimulation for treatment of hyperalgesia and pain. In Current Rheumatology Reports (Vol. 10, Issue 6, pp. 492–499). NIH Public Access. https://doi.org/10.1007/s11926-008-0080-z
- Dubinsky, R. M., & Miyasaki, J. (2010). Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): Report of the therapeutics and technology assessment subcommittee of the American academy of neurology. Neurology, 74(2), 173–176. https://doi.org/10.1212/WNL.0b013e3181c918fc
- Haldeman, S., Carroll, L., Cassidy, J. D., Schubert, J., & Nygren, Å. (2008). The Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders: Executive summary. In Spine (Vol. 33, Issue 4 SUPPL.). Spine (Phila Pa 1976). https://doi.org/10.1097/BRS.0b013e3181643f40
- Nnoaham, K. E., & Kumbang, J. (2008). Transcutaneous electrical nerve stimulation (TENS) for chronic pain. In Cochrane Database of Systematic Reviews (Issue 3). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD003222.pub2
- Ellrich, J., & Lamp, S. (2005). Peripheral nerve stimulation inhibits nociceptive processing: An electrophysiological study in healthy volunteers. Neuromodulation, 8(4), 225–232. https://doi.org/10.1111/j.1525-1403.2005.00029.x
- Rabago, D., Kijowski, R., Woods, M., Patterson, J. J., Mundt, M., Zgierska, A., Grettie, J., Lyftogt, J., & Fortney, L. (2013). Association between disease-specific quality of life and magnetic resonance imaging outcomes in a clinical trial of prolotherapy for knee osteoarthritis. Archives of Physical Medicine and Rehabilitation, 94(11), 2075–2082. https://doi.org/10.1016/j.apmr.2013.06.025
- Rabago, D., Best, T. M., Beamsley, M., & Patterson, J. (2005). A systematic review of prolotherapy for chronic musculoskeletal pain. In Clinical Journal of Sport Medicine (Vol. 15, Issue 5, pp. 376–380). Lippincott Williams and Wilkins. https://doi.org/10.1097/01.jsm.0000173268.05318.a4
- Sanderson, L. M., & Bryant, A. (2015). Effectiveness and safety of prolotherapy injections for management of lower limb tendinopathy and fasciopathy: A systematic review. In Journal of Foot and Ankle Research (Vol. 8, Issue 1, pp. 1–15). BioMed Central Ltd. https://doi.org/10.1186/s13047-015-0114-5
- Staal, J. B., De Bie, R. A., De Vet, H. C. W., Hildebrandt, J., & Nelemans, P. (2009). Injection therapy for subacute and chronic low back pain: An updated cochrane review. Spine, 34(1), 49–59. https://doi.org/10.1097/BRS.0b013e3181909558
- Kesikburun, S., Tan, A. K., Yilmaz, B., Yaşar, E., & Yazicioǧlu, K. (2013). Platelet-rich plasma injections in the treatment of chronic rotator cuff tendinopathy: A randomized controlled trial with 1-year follow-up. American Journal of Sports Medicine, 41(11), 2609–2615. https://doi.org/10.1177/0363546513496542
- Kim, S. R., Stitik, T. P., Foye, P. M., Greenwald, B. D., & Campagnolo, D. I. (2004). Critical Review of Prolotherapy for Osteoarthritis, Low Back Pain and other Musculoskeletal Conditions: A Physiatric Perspective. In American Journal of Physical Medicine and Rehabilitation (Vol. 83, Issue 5, pp. 379–389). Am J Phys Med Rehabil. https://doi.org/10.1097/01.PHM.0000124443.31707.74
- Hush, J. M., Cameron, K., & Mackey, M. (2011). Patient satisfaction with musculoskeletal physical therapy care: A systematic review. In Physical Therapy (Vol. 91, Issue 1, pp. 25–36). Oxford Academic. https://doi.org/10.2522/ptj.20100061
- Malliaras, P., Cook, J., Purdam, C., & Rio, E. (2015). Patellar tendinopathy: Clinical diagnosis, load management, and advice for challenging case presentations. In Journal of Orthopaedic and Sports Physical Therapy (Vol. 45, Issue 11, pp. 887–898). Movement Science Media. https://doi.org/10.2519/jospt.2015.5987
- van der Heijden, R. A., Lankhorst, N. E., van Linschoten, R., Bierma-Zeinstra, S. M., & van Middelkoop, M. (2015). Exercise for treating patellofemoral pain syndrome. In Cochrane Database of Systematic Reviews (Vol. 2017, Issue 6). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD010387.pub2
- Bleakley, C., McDonough, S., & MacAuley, D. (2004). The Use of Ice in the Treatment of Acute Soft-Tissue Injury: A Systematic Review of Randomized Controlled Trials. In American Journal of Sports Medicine (Vol. 32, Issue 1, pp. 251–261). SAGE Publications Inc. https://doi.org/10.1177/0363546503260757
- Hing, W. A., White, S. G., Bouaaphone, A., & Lee, P. (2008). Contrast therapy-A systematic review. In Physical Therapy in Sport (Vol. 9, Issue 3, pp. 148–161). Phys Ther Sport. https://doi.org/10.1016/j.ptsp.2008.06.001
- Malanga, G. A., Yan, N., & Stark, J. (2015). Mechanisms and efficacy of heat and cold therapies for musculoskeletal injury. In Postgraduate Medicine (Vol. 127, Issue 1, pp. 57–65). Taylor and Francis Inc. https://doi.org/10.1080/00325481.2015.992719
- Collins, N. C. (2008). Is ice right? Does cryotherapy improve outcome for acute soft tissue injury? In Emergency Medicine Journal (Vol. 25, Issue 2, pp. 65–68). Emerg Med J. https://doi.org/10.1136/emj.2007.051664
- Wandel, S., Jüni, P., Tendal, B., Nüesch, E., Villiger, P. M., Welton, N. J., Reichenbach, S., & Trelle, S. (2010). Effects of glucosamine, chondroitin, or placebo in patients with osteoarthritis of hip or knee: Network meta-analysis. BMJ (Online), 341(7775), 711. https://doi.org/10.1136/bmj.c4675
- Sawitzke, A. D., Shi, H., Finco, M. F., Dunlop, D. D., Harris, C. L., Singer, N. G., Bradley, J. D., Silver, D., Jackson, C. G., Lane, N. E., Oddis, C. V., Wolfe, F., Lisse, J., Furst, D. E., Bingham, C. O., Reda, D. J., Moskowitz, R. W., Williams, H. J., & Clegg, D. O. (2010). Clinical efficacy and safety of glucosamine, chondroitin sulphate, their combination, celecoxib or placebo taken to treat osteoarthritis of the knee: 2-Year results from GAIT. Annals of the Rheumatic Diseases, 69(8), 1459–1464. https://doi.org/10.1136/ard.2009.120469
- Wilkens, P., Scheel, I. B., Grundnes, O., Hellum, C., & Storheim, K. (2010). Effect of glucosamine on pain-related disability in patients with chronic low back pain and degenerative lumbar osteoarthritis: A randomized controlled trial. JAMA - Journal of the American Medical Association, 304(1), 45–52. https://doi.org/10.1001/jama.2010.893
- Clegg, D. O., Reda, D. J., Harris, C. L., Klein, M. A., O’Dell, J. R., Hooper, M. M., Bradley, J. D., Bingham, C. O., Weisman, M. H., Jackson, C. G., Lane, N. E., Cush, J. J., Moreland, L. W., Schumacher, H. R., Oddis, C. V., Wolfe, F., Molitor, J. A., Yocum, D. E., Schnitzer, T. J., … Williams, H. J. (2006). Glucosamine, Chondroitin Sulfate, and the Two in Combination for Painful Knee Osteoarthritis. New England Journal of Medicine, 354(8), 795–808. https://doi.org/10.1056/nejmoa052771
- Ong, C. K. S., Lirk, P., Tan, C. H., & Seymour, R. A. (2007). An evidence-based update on nonsteroidal anti-inflammatory drugs. In Clinical Medicine and Research (Vol. 5, Issue 1, pp. 19–34). Marshfield Clinic. https://doi.org/10.3121/cmr.2007.698
- Enthoven, W. T. M., Roelofs, P. D. D. M., Deyo, R. A., van Tulder, M. W., & Koes, B. W. (2016). Non-steroidal anti-inflammatory drugs for chronic low back pain. In Cochrane Database of Systematic Reviews (Vol. 2016, Issue 2). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD012087
- Derry, S., Moore, R. A., Gaskell, H., Mcintyre, M., & Wiffen, P. J. (2015). Topical NSAIDs for acute musculoskeletal pain in adults. In Cochrane Database of Systematic Reviews (Vol. 2017, Issue 3). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD007402.pub3
- Lun, V., Meeuwisse, W. H., Stergiou, P., & Stefanyshyn, D. (2004). Relation between running injury and static lower limb alignment in recreational runners. British Journal of Sports Medicine, 38(5), 576–580. https://doi.org/10.1136/bjsm.2003.005488
- Hides J, Fan T, Stanton W, Stanton P, McMahon K, & Wilson S. (n.d.). Asymmetry of psoas and quadratus lumborum unrelated to injury. Retrieved June 3, 2021, from https://www.painscience.com/biblio/asymmetry-of-psoas-and-quadratus-lumborum-unrelated-to-injury.html
- Finan, P. H., Buenaver, L. F., Bounds, S. C., Hussain, S., Park, R. J., Haque, U. J., Campbell, C. M., Haythornthwaite, J. A., Edwards, R. R., & Smith, M. T. (2013). Discordance between pain and radiographic severity in knee osteoarthritis: Findings from quantitative sensory testing of central sensitization. Arthritis and Rheumatism, 65(2), 363–372. https://doi.org/10.1002/art.34646
- Moseley, G. L. (2012). Teaching people about pain: why do we keep beating around the bush? Pain Management, 2(1), 1–3. https://doi.org/10.2217/pmt.11.73
- Zusman, M. (2011). The Modernisation of Manipulative Therapy. International Journal of Clinical Medicine, 02(05), 644–649. https://doi.org/10.4236/ijcm.2011.25110
- Dye, S. F. (2005). The pathophysiology of patellofemoral pain: A tissue homeostasis perspective. Clinical Orthopaedics and Related Research, 436, 100–110. https://doi.org/10.1097/01.blo.0000172303.74414.7d
- Lederman, E. (n.d.). Fall of PSB model in manual and physical therapies. Retrieved June 3, 2021, from https://www.cpdo.net/Lederman_The_fall_of_the_postural-structural-biomechanical_model.pdf
- Bliddal, H., Leeds, A. R., & Christensen, R. (2014). Osteoarthritis, obesity and weight loss: Evidence, hypotheses and horizons - a scoping review. Obesity Reviews, 15(7), 578–586. https://doi.org/10.1111/obr.12173
- Forsythe, L. K., Wallace, J. M. W., & Livingstone, M. B. E. (2008). Obesity and inflammation: The effects of weight loss. Nutrition Research Reviews, 21(2), 117–133. https://doi.org/10.1017/S0954422408138732
- Sokolove, J., & Lepus, C. M. (2013). Role of inflammation in the pathogenesis of osteoarthritis: Latest findings and interpretations. Therapeutic Advances in Musculoskeletal Disease, 5(2), 77–94. https://doi.org/10.1177/1759720X12467868
- Neogi, T., Guermazi, A., Roemer, F., Nevitt, M. C., Scholz, J., Arendt-Nielsen, L., Woolf, C., Niu, J., Bradley, L. A., Quinn, E., & Frey Law, L. (2016). Association of Joint Inflammation with Pain Sensitization in Knee Osteoarthritis: The Multicenter Osteoarthritis Study. Arthritis and Rheumatology, 68(3), 654–661. https://doi.org/10.1002/art.39488
- Gregor, M. F., & Hotamisligil, G. S. (2011). Inflammatory mechanisms in obesity. Annual Review of Immunology, 29, 415–445. https://doi.org/10.1146/annurev-immunol-031210-101322
- Rechardt, M., Shiri, R., Karppinen, J., Jula, A., Heliövaara, M., & Viikari-Juntura, E. (2010). Lifestyle and metabolic factors in relation to shoulder pain and rotator cuff tendinitis: A population-based study. BMC Musculoskeletal Disorders, 11, 165. https://doi.org/10.1186/1471-2474-11-165
- Yusuf, E., Nelissen, R. G., Ioan-Facsinay, A., Stojanovic-Susulic, V., DeGroot, J., Van Osch, G., Middeldorp, S., Huizinga, T. W. J., & Kloppenburg, M. (2010). Association between weight or body mass index and hand osteoarthritis: A systematic review. Annals of the Rheumatic Diseases, 69(4), 761–765. https://doi.org/10.1136/ard.2008.106930
- Carman, W. J., Sowers, M., Hawthorne, V. M., & Weissfeld, L. A. (1994). Obesity as a risk factor for osteoarthritis of the hand and wrist: A prospective study. American Journal of Epidemiology, 139(2), 119–129. https://doi.org/10.1093/oxfordjournals.aje.a116974
- Felson, D. T., Zhang, Y., Hannan, M. T., Naimark, A., Weissman, B., Aliabadi, P., & Levy, D. (1997). Risk factors for incident radiographic knee osteoarthritis in the elderly. Arthritis and Rheumatism, 40(4), 728–733. https://doi.org/10.1002/art.1780400420
- Messier, S. P., Gutekunst, D. J., Davis, C., & DeVita, P. (2005). Weight loss reduces knee-joint loads in overweight and obese older adults with knee osteoarthritis. Arthritis and Rheumatism, 52(7), 2026–2032. https://doi.org/10.1002/art.21139
- Loeser, R. F. (2006). Molecular mechanisms of cartilage destruction: Mechanics, inflammatory mediators, and aging collide. In Arthritis and Rheumatism (Vol. 54, Issue 5, pp. 1357–1360). NIH Public Access. https://doi.org/10.1002/art.21813
- Anderson, J. J., & Felson, D. T. (1988). Factors associated with osteoarthritis of the knee in the first national health and nutrition examination survey (Hanes I): Evidence for an association with overweight, race, and physical demands of work. American Journal of Epidemiology, 128(1), 179–189. https://doi.org/10.1093/oxfordjournals.aje.a114939
- Messier, S. P. (2010). Diet and exercise for obese adults with knee osteoarthritis. In Clinics in Geriatric Medicine (Vol. 26, Issue 3, pp. 461–477). NIH Public Access. https://doi.org/10.1016/j.cger.2010.05.001
- Smith, S. M., Sumar, B., & Dixon, K. A. (2014). Musculoskeletal pain in overweight and obese children. In International Journal of Obesity (Vol. 38, Issue 1, pp. 11–15). Nature Publishing Group. https://doi.org/10.1038/ijo.2013.187
- Schouten, J. S. A. G., Van Den Ouweland, F. A., & Valkenburg, H. A. (1992). A 12 year follow up study in the general population on prognostic factors of cartilage loss in osteoarthritis of the knee. Annals of the Rheumatic Diseases, 51(8), 932–937. https://doi.org/10.1136/ard.51.8.932
- Messier, S. P., Legault, C., Schoenlank, C. R., Newman, J. J., Martin, D. F., & Devita, P. (2008). Risk factors and mechanisms of knee injury in runners. Medicine and Science in Sports and Exercise, 40(11), 1873–1879. https://doi.org/10.1249/MSS.0b013e31817ed272
- Madsen, M. V., Gøtzsche, P. C., & Hróbjartsson, A. (2009). Acupuncture treatment for pain: Systematic review of randomised clinical trials with acupuncture, placebo acupuncture, and no acupuncture groups. BMJ (Online), 338(7690), 330–333. https://doi.org/10.1136/bmj.a3115
- Manheimer, E., Cheng, K., Linde, K., Lao, L., Yoo, J., Wieland, S., van der Windt, D. A., Berman, B. M., & Bouter, L. M. (2010). Acupuncture for peripheral joint osteoarthritis. Cochrane Database of Systematic Reviews. https://doi.org/10.1002/14651858.cd001977.pub2
- Hróbjartsson, A., & Gøtzsche, P. C. (2010). Placebo interventions for all clinical conditions. In Cochrane Database of Systematic Reviews (Vol. 2010, Issue 1). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD003974.pub3
- Karanicolas, P. J., Farrokhyar, F., & Bhandari, M. (2010). Blinding: Who, what, when, why, how? Canadian Journal of Surgery, 53(5), 345–348. /pmc/articles/PMC2947122/
- Casimiro, L., Barnsley, L., Brosseau, L., Milne, S., Welch, V., Tugwell, P., & Wells, G. A. (2005). Acupuncture and electroacupuncture for the treatment of rheumatoid arthritis. Cochrane Database of Systematic Reviews. https://doi.org/10.1002/14651858.cd003788.pub2
- Colquhoun, D., & Novella, S. P. (2013). Acupuncture is theatrical placebo. In Anesthesia and Analgesia (Vol. 116, Issue 6, pp. 1360–1363). Anesth Analg. https://doi.org/10.1213/ANE.0b013e31828f2d5e
- Zhang, Q., Yue, J., Golianu, B., Sun, Z., & Lu, Y. (2017). Updated systematic review and meta-analysis of acupuncture for chronic knee pain. In Acupuncture in Medicine (Vol. 35, Issue 6, pp. 392–403). BMJ Publishing Group. https://doi.org/10.1136/acupmed-2016-011306
- White, A., Foster, N. E., Cummings, M., & Barlas, P. (2007). Acupuncture treatment for chronic knee pain: A systematic review. In Rheumatology (Vol. 46, Issue 3, pp. 384–390). Rheumatology (Oxford). https://doi.org/10.1093/rheumatology/kel413
- Vickers, A. J., Cronin, A. M., Maschino, A. C., Lewith, G., MacPherson, H., Foster, N. E., Sherman, K. J., Witt, C. M., & Linde, K. (2012). Acupuncture for chronic pain: Individual patient data meta-analysis. In Archives of Internal Medicine (Vol. 172, Issue 19, pp. 1444–1453). American Medical Association. https://doi.org/10.1001/archinternmed.2012.3654
- Rathbone, A. T. L., Grosman-Rimon, L., & Kumbhare, D. A. (2017). Interrater Agreement of Manual Palpation for Identification of Myofascial Trigger Points: A Systematic Review and Meta-Analysis. In Clinical Journal of Pain (Vol. 33, Issue 8, pp. 715–729). Lippincott Williams and Wilkins. https://doi.org/10.1097/AJP.0000000000000459
- F Wolfe, D G Simons, J Fricton, R M Bennett, D L Goldenberg, R Gerwin, D Hathaway, G A McCain, I J Russell, & H O Sanders. (n.d.). The fibromyalgia and myofascial pain syndromes: a preliminary study of tender points and trigger points in persons with fibromyalgia, myofascial pain syndrome and no disease - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/1404132/
- Andersen, H., Ge, H. Y., Arendt-Nielsen, L., Danneskiold-Samsøe, B., & Graven-Nielsen, T. (2010). Increased Trapezius Pain Sensitivity Is Not Associated With Increased Tissue Hardness. Journal of Pain, 11(5), 491–499. https://doi.org/10.1016/j.jpain.2009.09.017
- Ajimsha, M. S., Al-Mudahka, N. R., & Al-Madzhar, J. A. (2015). Effectiveness of myofascial release: Systematic review of randomized controlled trials. Journal of Bodywork and Movement Therapies, 19(1), 102–112. https://doi.org/10.1016/j.jbmt.2014.06.001
- Chaibi, A., Benth, J., Tuchin, P. J., & Russell, M. B. (2017). Chiropractic spinal manipulative therapy for migraine: a three-armed, single-blinded, placebo, randomized controlled trial. European Journal of Neurology, 24(1), 143–153. https://doi.org/10.1111/ene.13166
- Background - Selective Outcome Reporting as a Source of Bias in Reviews of Comparative Effectiveness - NCBI Bookshelf. (n.d.). Retrieved June 3, 2021, from https://www.ncbi.nlm.nih.gov/books/NBK100617/
- Faber, J., & Fonseca, L. M. (2014). How sample size influences research outcomes. Dental Press Journal of Orthodontics, 19(4), 27–29. https://doi.org/10.1590/2176-9451.19.4.027-029.ebo
- Rubinstein, S. M., Terwee, C. B., Assendelft, W. J., de Boer, M. R., & van Tulder, M. W. (2012). Spinal manipulative therapy for acute low-back pain. Cochrane Database of Systematic Reviews. https://doi.org/10.1002/14651858.cd008880.pub2
- Hoskins, W. T., & Polland, H. P. (2005). Successful management of hamstring injuries in Australian Rules footballers: Two case reports. Chiropractic and Osteopathy, 13(1). https://doi.org/10.1186/1746-1340-13-4
- Pollard, H., Ward, G., Hoskins, W., & Hardy, K. (2008). The effect of a manual therapy knee protocol on osteoarthritic knee pain: a randomised controlled trial. The Journal of the Canadian Chiropractic Association, 52(4), 229–242. http://www.ncbi.nlm.nih.gov/pubmed/19066697
- Mirtz, T. A., Morgan, L., Wyatt, L. H., & Greene, L. (2009). An epidemiological examination of the subluxation construct using Hill’s criteria of causation. In Chiropractic and Osteopathy (Vol. 17, p. 13). BioMed Central. https://doi.org/10.1186/1746-1340-17-13
- Hoskins, W., McHardy, A., Pollard, H., Windsham, R., & Onley, R. (2006). Chiropractic Treatment of Lower Extremity Conditions: a Literature Review. In Journal of Manipulative and Physiological Therapeutics (Vol. 29, Issue 8, pp. 658–671). J Manipulative Physiol Ther. https://doi.org/10.1016/j.jmpt.2006.08.004
- Walker, B. F., French, S. D., Grant, W., & Green, S. (2011). A cochrane review of combined chiropractic interventions for low-back pain. In Spine (Vol. 36, Issue 3, pp. 230–242). Spine (Phila Pa 1976). https://doi.org/10.1097/BRS.0b013e318202ac73
- Rubinstein, S. M., Middelkoop, M. van, Assendelft, W. J., Boer, M. R. de, & Tulder, M. W. van. (2011). Spinal manipulative therapy for chronic low back pain. In Drug and Therapeutics Bulletin (Vol. 49, Issue 4, p. 41). John Wiley & Sons, Ltd. https://doi.org/10.1002/14651858.cd008112.pub2
- Sagheer, M. A., Khan, M. F., & Sharif, S. (n.d.). Association between chronic low back pain, anxiety and depression in patients at a tertiary care centre - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/23901665/
- Moyer, C. A. (n.d.). Affective massage therapy - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/21589715/
- Webb, T. R., & Rajendran, D. (2016). Myofascial techniques: What are their effects on joint range of motion and pain? – A systematic review and meta-analysis of randomised controlled trials. Journal of Bodywork and Movement Therapies, 20(3), 682–699. https://doi.org/10.1016/j.jbmt.2016.02.013
- Fitzgerald, B., & McLatchie, G. R. (1980). Degenerative joint disease in weight-lifters. Fact or fiction? British Journal of Sports Medicine, 14(2–3), 97–101. https://doi.org/10.1136/bjsm.14.2-3.97
- Steiner, M. E., Grana, W. A., Chillag, K., & Schelberg-Karnes, E. (1986). The effect of exercise on anterior-posterior knee laxity. The American Journal of Sports Medicine, 14(1), 24–29. https://doi.org/10.1177/036354658601400105
- Chandler, T. J., Wilson, G. D., & Stone, M. H. (n.d.). The effect of the squat exercise on knee stability - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/2733579/
- Escamilla, R. F., Fleisig, G. S., Zheng, N., Lander, J. E., Barrentine, S. W., Andrews, J. R., Bergemann, B. W., & Moorman, C. T. (2001). Effects of technique variations on knee biomechanics during the squat and leg press. Medicine and Science in Sports and Exercise, 33(9), 1552–1566. https://doi.org/10.1097/00005768-200109000-00020
- Gullett, J. C., Tillman, M. D., Gutierrez, G. M., & Chow, J. W. (2009). A biomechanical comparison of back and front squats in healthy trained individuals. Journal of Strength and Conditioning Research, 23(1), 284–292. https://doi.org/10.1519/JSC.0b013e31818546bb
- Toutoungi, D. E., Lu, T. W., Leardini, A., Catani, F., & O’Connor, J. J. (2000). Cruciate ligament forces in the human knee during rehabilitation exercises. Clinical Biomechanics, 15(3), 176–187. https://doi.org/10.1016/S0268-0033(99)00063-7
- Escamilla, R. F. (2001). Knee biomechanics of the dynamic squat exercise. Medicine and Science in Sports and Exercise, 33(1), 127–141. https://doi.org/10.1097/00005768-200101000-00020
- Michels, F., Jambou, S., Allard, M., Bousquet, V., Colombet, P., & De Lavigne, C. (2009). An arthroscopic technique to treat the iliotibial band syndrome. Knee Surgery, Sports Traumatology, Arthroscopy, 17(3), 233–236. https://doi.org/10.1007/s00167-008-0660-5
- Muhle, C., Ahn, J. M., Yeh, L. R., Bergman, G. A., Boutin, R. D., Schweitzer, M., Jacobson, J. A., Haghighi, P., Trudell, D. J., & Resnick, D. (1999). Iliotibial band friction syndrome: MR imaging findings in 16 patients and MR arthrographic study of six cadaveric knees. Radiology, 212(1), 103–110. https://doi.org/10.1148/radiology.212.1.r99jl29103
- Langevin, H. M., Stevens-Tuttle, D., Fox, J. R., Badger, G. J., Bouffard, N. A., Krag, M. H., Wu, J., & Henry, S. M. (2009). Ultrasound evidence of altered lumbar connective tissue structure in human subjects with chronic low back pain. BMC Musculoskeletal Disorders, 10(1). https://doi.org/10.1186/1471-2474-10-151
- Berrueta, L., Muskaj, I., Olenich, S., Butler, T., Badger, G. J., Colas, R. A., Spite, M., Serhan, C. N., & Langevin, H. M. (2016). Stretching Impacts Inflammation Resolution in Connective Tissue. Journal of Cellular Physiology, 231(7), 1621–1627. https://doi.org/10.1002/jcp.25263
- Kim, J. H., Lee, H. S., & Park, S. W. (2015). Effects of the active release technique on pain and range of motion of patients with chronic neck pain. Journal of Physical Therapy Science, 27(8), 2461–2464. https://doi.org/10.1589/jpts.27.2461
- Sherman, K. J., Cherkin, D. C., Wellman, R. D., Cook, A. J., Hawkes, R. J., Delaney, K., & Deyo, R. A. (2011). A randomized trial comparing yoga, stretching, and a self-care book for chronic low back pain. Archives of Internal Medicine, 171(22), 2019–2026. https://doi.org/10.1001/archinternmed.2011.524
- Sherman, K. J., Cherkin, D. C., Cook, A. J., Hawkes, R. J., Deyo, R. A., Wellman, R., & Khalsa, P. S. (2010). Comparison of yoga versus stretching for chronic low back pain: Protocol for the Yoga Exercise Self-care (YES) trial. Trials, 11, 36. https://doi.org/10.1186/1745-6215-11-36
- Herbert, R. D., & Gabriel, M. (2002). Effects of stretching before and after exercising on muscle soreness and risk of injury: Systematic review. In British Medical Journal (Vol. 325, Issue 7362, pp. 468–470). British Medical Journal Publishing Group. https://doi.org/10.1136/bmj.325.7362.468
- Pope, R. P., Herbert, R. D., Kirwan, J. D., & Graham, B. J. (2000). A randomized trial of preexercise stretching for prevention of lower- limb injury. Medicine and Science in Sports and Exercise, 32(2), 271–277. https://doi.org/10.1097/00005768-200002000-00004
- Eng, C. M., Arnold, A. S., Lieberman, D. E., & Biewener, A. A. (2015). The capacity of the human iliotibial band to store elastic energy during running. Journal of Biomechanics, 48(12), 3341–3348. https://doi.org/10.1016/j.jbiomech.2015.06.017
- Fairclough, J., Hayashi, K., Toumi, H., Lyons, K., Bydder, G., Phillips, N., Best, T. M., & Benjamin, M. (2006). The functional anatomy of the iliotibial band during flexion and extension of the knee: Implications for understanding iliotibial band syndrome. Journal of Anatomy, 208(3), 309–316. https://doi.org/10.1111/j.1469-7580.2006.00531.x
- Willett, G. M., Keim, S. A., Shostrom, V. K., & Lomneth, C. S. (2016). An Anatomic Investigation of the Ober Test. American Journal of Sports Medicine, 44(3), 696–701. https://doi.org/10.1177/0363546515621762
- Fairclough, J., Hayashi, K., Toumi, H., Lyons, K., Bydder, G., Phillips, N., Best, T. M., & Benjamin, M. (2007). Is iliotibial band syndrome really a friction syndrome? In Journal of Science and Medicine in Sport (Vol. 10, Issue 2, pp. 74–76). Sports Medicine Australia. https://doi.org/10.1016/j.jsams.2006.05.017
- Knapik, J. J., Bauman, C. L., Jones, B. H., Harris, J. M., & Vaughan, L. (1991). Preseason strength and flexibility imbalances associated with athletic injuries in female collegiate athletes. American Journal of Sports Medicine, 19(1), 76–81. https://doi.org/10.1177/036354659101900113
- Vincent, K. R., & Vincent, H. K. (2012). Resistance Exercise for Knee Osteoarthritis. PM and R, 4(5 SUPPL.), S45. https://doi.org/10.1016/j.pmrj.2012.01.019
- Smith, T. O., Davies, L., & Donell, S. T. (2009). The reliability and validity of assessing medio-lateral patellar position: a systematic review. In Manual Therapy (Vol. 14, Issue 4, pp. 355–362). Man Ther. https://doi.org/10.1016/j.math.2008.08.001
- MacIntyre, N. J., Hill, N. A., Fellows, R. A., Ellis, R. E., & Wilson, D. R. (2006). Patellofemoral joint kinematics in individuals with and without patellofemoral pain syndrome. Journal of Bone and Joint Surgery - Series A, 88(12), 2596–2605. https://doi.org/10.2106/JBJS.E.00674
- Tennant, S., Williams, A., Vedi, V., Kinmont, C., Gedroyc, W., & Hunt, D. M. (2001). Patello-femoral tracking in the weight-bearing knee: A study of asymptomatic volunteers utilising dynamic magnetic resonance imaging: A preliminary report. Knee Surgery, Sports Traumatology, Arthroscopy, 9(3), 155–162. https://doi.org/10.1007/s001670000173
- Lee, T. Q., Sandusky, M. D., Adeli, A., & McMahon, P. J. (n.d.). Effects of simulated vastus medialis strength variation on patellofemoral joint biomechanics in human cadaver knees - PubMed. Retrieved June 3, 2021, from https://pubmed.ncbi.nlm.nih.gov/12173763/
- Peeler, J., & Anderson, J. E. (2007). Structural parameters of the vastus medialis muscles and its relationship to patellofemoral joint deterioration. Clinical Anatomy, 20(3), 307–314. https://doi.org/10.1002/ca.20375
- Gifstad, T., Sole, A., Strand, T., Uppheim, G., Grøntvedt, T., & Drogset, J. O. (2013). Long-term follow-up of patellar tendon grafts or hamstring tendon grafts in endoscopic ACL reconstructions. Knee Surgery, Sports Traumatology, Arthroscopy, 21(3), 576–583. https://doi.org/10.1007/s00167-012-1947-0
- Kise, N. J., Risberg, M. A., Stensrud, S., Ranstam, J., Engebretsen, L., & Roos, E. M. (2016). Exercise therapy versus arthroscopic partial meniscectomy for degenerative meniscal tear in middle aged patients: Randomised controlled trial with two year follow-up. The BMJ, 354. https://doi.org/10.1136/bmj.i3740
- Thorlund, J. B., Juhl, C. B., Roos, E. M., & Lohmander, L. S. (2015). Arthroscopic surgery for degenerative knee: Systematic review and meta-analysis of benefits and harms. In BMJ (Online) (Vol. 350). BMJ Publishing Group. https://doi.org/10.1136/bmj.h2747
- Sihvonen, R., Paavola, M., Malmivaara, A., Itälä, A., Joukainen, A., Nurmi, H., Kalske, J., & Järvinen, T. L. N. (2013). Arthroscopic Partial Meniscectomy versus Sham Surgery for a Degenerative Meniscal Tear. New England Journal of Medicine, 369(26), 2515–2524. https://doi.org/10.1056/nejmoa1305189
- Louw, A., Diener, I., Fernández-de-Las-Peñas, C., & Puentedura, E. J. (2017). Sham Surgery in Orthopedics: A Systematic Review of the Literature. Pain Medicine (Malden, Mass.), 18(4), 736–750. https://doi.org/10.1093/pm/pnw164
- Kirkley, A., Birmingham, T. B., Litchfield, R. B., Giffin, J. R., Willits, K. R., Wong, C. J., Feagan, B. G., Donner, A., Griffin, S. H., D’Ascanio, L. M., Pope, J. E., & Fowler, P. J. (2008). A Randomized Trial of Arthroscopic Surgery for Osteoarthritis of the Knee. New England Journal of Medicine, 359(11), 1097–1107. https://doi.org/10.1056/NEJMoa0708333
- Siemieniuk, R. A. C., Harris, I. A., Agoritsas, T., Poolman, R. W., Brignardello-Petersen, R., Van De Velde, S., Buchbinder, R., Englund, M., Lytvyn, L., Quinlan, C., Helsingen, L., Knutsen, G., Olsen, N. R., MacDonald, H., Hailey, L., Wilson, H. M., Lydiatt, A., & Kristiansen, A. (2017). Arthroscopic surgery for degenerative knee arthritis and meniscal tears: A clinical practice guideline. BMJ (Online), 357. https://doi.org/10.1136/bmj.j1982
- Johnson, L. L. (2002). A controlled trial of arthroscopic surgery for osteoarthritis of the knee. In Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association (Vol. 18, Issue 7, pp. 683–687). Massachusetts Medical Society . https://doi.org/10.1056/nejmoa013259
- Laupattarakasem, W., Laopaiboon, M., Laupattarakasem, P., & Sumananont, C. (2008). Arthroscopic debridement for knee osteoarthritis. In Cochrane Database of Systematic Reviews (Issue 1). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD005118.pub2
- Sophia Fox, A. J., Bedi, A., & Rodeo, S. A. (2009). The basic science of articular cartilage: Structure, composition, and function. Sports Health, 1(6), 461–468. https://doi.org/10.1177/1941738109350438
- Guenther, K. (2016). “It’s All Done with Mirrors”: V.S. Ramachandran and the Material Culture of Phantom Limb Research. In Medical History (Vol. 60, Issue 3, pp. 342–358). Cambridge University Press. https://doi.org/10.1017/mdh.2016.27
- Patel, D. R., Yamasaki, A., & Brown, K. (2017). Epidemiology of sports-related musculoskeletal injuries in young athletes in United States. In Translational Pediatrics (Vol. 6, Issue 3, pp. 160–166). AME Publishing Company. https://doi.org/10.21037/tp.2017.04.08
- Patel, D. R., & Villalobos, A. (2017). Evaluation and management of knee pain in young athletes: Overuse injuries of the knee. In Translational Pediatrics (Vol. 6, Issue 3, pp. 190–198). AME Publishing Company. https://doi.org/10.21037/tp.2017.04.05
- van Mechelen, W. (1992). Running Injuries: A Review of the Epidemiological Literature. In Sports Medicine: An International Journal of Applied Medicine and Science in Sport and Exercise (Vol. 14, Issue 5, pp. 320–335). Sports Med. https://doi.org/10.2165/00007256-199214050-00004
- Clarsen, B., Krosshaug, T., & Bahr, R. (2010). Overuse injuries in professional road cyclists. American Journal of Sports Medicine, 38(12), 2494–2501. https://doi.org/10.1177/0363546510376816
- Nguyen, U. S. D. T., Zhang, Y., Zhu, Y., Niu, J., Zhang, B., & Felson, D. T. (2011). Increasing prevalence of knee pain and symptomatic knee osteoarthritis: Survey and cohort data. Annals of Internal Medicine, 155(11), 725–732. https://doi.org/10.7326/0003-4819-155-11-201112060-00004












