Key Takeaways
- Regardless of how good the rest of your habits are, having more body fat increases your chances of many health problems.
- Exercising and eating a healthy diet can reduce your risk of these problems, regardless of whether or not you’re overweight, but it can’t completely prevent them.
- The point where exercise and diet can offset the negative effects of obesity is higher than many people think, but the bottom line is that leaner people are generally healthier.
Losing weight is hard.
If you don’t agree with that now then spend some time in a gym and meet a few hundred people who do think that. Sometimes you diet and exercise and nothing happens.
It gets frustrating at times, knowing that all the hard work you put into changing your body amounted to absolutely nothing.
What if you don’t really need to lose weight to be healthy?
More and more people are saying that being overweight isn’t necessarily what leads to ill health. It’s just lack of exercise, poor diet, high stress, and other unhealthy habits.
This idea is part of a growing movement known as “health at every size,” that states that instead of focusing on weight, people should just focus on eating better, moving more, and practicing good habits, regardless of the outcome.
Other people say that, no, your weight does matter, and one of the single best ways to improve your health, live longer, and feel better is to lose weight.
Who’s right?
Well, the short story is that being overweight or obese is, by definition, unhealthy. The good news, though, is that the amount of body fat it takes to negatively affect your health is probably higher than you might think, and you can keep many of the problems at bay by eating right and exercising.
In this article, you’re going to learn what a healthy weight really is, whether or not exercise and diet can offset the negative effects of being overweight, and when you absolutely should lose weight regardless of how good your other habits are.
- What Is a “Healthy” Weight?
- Can I Be Healthy when Overweight?
- Is Exercise Enough Without Weight Loss?
- When Should You Lose Weight?
- The Bottom Line on Fitness vs. Fatness
Table of Contents
+
Want to listen to more stuff like this? Check out my podcast!
What Is a “Healthy” Weight?
Right, so “healthy weight” is surprisingly hard to define. Different people have different definitions of it yet nobody tries to break it down to get everybody on the same page.
First, we need to define what “healthy” means. For the purpose of this article we’re going to be a bit loose with this term. Normally, I lean toward the biological definition of health, where a system in the body is “healthy” if it can function at full capacity and “unhealthy” if it can’t.
For example, person A has low HbA1c (a sign they process glucose well and have a low risk of diabetes) and person B has elevated HbA1c. Which one is healthier? I don’t know, I don’t care, neither of them have type II diabetes.
Person C, on the other hand, has type II diabetes so their glucose metabolism is, you could objectively say, “unhealthy.”
Sure, person B is “closer to unhealthy” than person A based on our chosen biomarker here (HbA1c), but they’re both fine and dandy; genetics can influence these numbers, too, and they often throw a monkey wrench in our plans of basing health on one or two numbers.
So when we talk about health, we’re talking about there not being any apparent disease states that impair the function of organs. Healthy people can operate as normal even in bad conditions and unhealthy people have faults in one or more systems.
Do note that the above isn’t talking about happiness, well being, or even comfort. Those aren’t the topics I want to cover in this article, I simply want to talk about risk of disease states and/or death.
That’s a major reason why the majority of people exercise anyways. They just don’t want to die quickly and, even if they don’t mind an early death, they’d rather die on their feet with good mobility and no diseases rather than in a hospital bed on tons of medication.
Anyways, rambling . . .
To get back on topic, now that we’re on the same page when it comes to what “healthy” means, a “healthy weight” simply means the weight that is best suited for not getting any disease states.
Generally speaking this is a body mass index (BMI) of 18.5 to 24.9, otherwise known as the “normal” weight range.
A BMI of 25 to 29.9 is in the “overweight” range and, while technically at an elevated risk for disease states, honestly isn’t that much of a big deal in terms of health and longevity.
This is especially true for athletes since the BMI was not made for us in the first place and doesn’t assume a high level of muscle tissue. I’d wager a bet that many of the athletes that you look up to are in the overweight category yet are in the peak of health.
A BMI of 30 to 34.9 is in the “obese” range. As soon as you pass 30 then risk of diseases goes up to a level that’s actually a concern. This’s when your doctor is going to start suggesting weight loss.
A BMI of 35+ is in the “morbid obesity” range. Like, come on, it has morbid in the name. For good reason too, as the risk of many diseases shoots up when BMI passes this stage and weight loss becomes one of the most important things to aim for.
After breaking into the “morbid obesity” range, higher and higher weights are ranked on different levels, like leveling up in a video game. For example, “morbid obesity class lll” means you have a BMI of over 40. After that they stop counting.
This is where things get really bad.
That being said, if losing weight was easy then we wouldn’t have an obesity epidemic. Weight loss is simple in theory, and it’s simple to make a plan, but difficult for many people to execute that plan.
There are a lot of people who make healthier changes to their diet and exercise, but still don’t lose any weight.
And yet, they do get some health benefits from it.
Is that enough, though? Even if you didn’t lose weight, were your efforts futile or did they bear fruit?
In other words, can you be healthy when you’re slightly or severely overweight if you get the other things right?
Can I Be Healthy when Overweight?
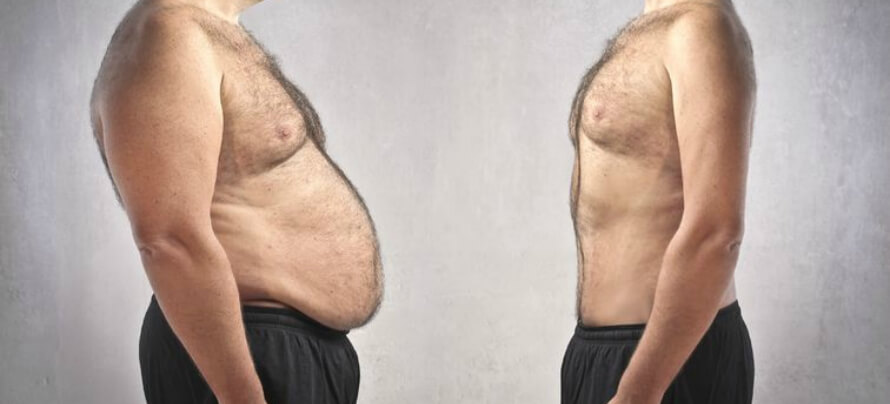
If you’ve been somewhat into health and wellness for some time, you may know of the “Health at Every Size” movement (HAES). You tend to see this acronym thrown around by obese people to validate their obesity.
Ironically, it had its scientific roots as a weight loss intervention and it’s actually pretty damn nice for improving quality of life, and often results in weight loss.
It’s a specialized dietary plan, aimed towards people who hyperfocus on their weight as an absolute number, and are prone to bouncing up and down in weight while jumping from fad diet to fad diet.
By thinking of your weight as nothing more than a number, focusing on the quality of food, and learning intuitive eating, weight loss actually occurs. Some variants of HAES actually have community involvement as well (getting a bunch of people to lose weight together) which is just superb.
Anything that focuses on community involvement and happiness tends to have great long-term results which are sorely needed for diet and exercise. It’s also why P90X and CrossFit have helped so many people, it got them together and gave them a reason to come back time and time again.
Unfortunately, the HAES acronym has been hijacked as a way to rationalize away the very real dangers of being overweight.
Now, it’s often used to validate poor eating choices and lack of self-control, and the idea that exercise and diet are the ONLY factors that affect health and that weight is irrelevant.
Does exercise matter? Yes.
Does diet matter? Absolutely.
Does weight matter? Less than the other two up to a point, but still yes.
By how much though? Well, that’s what spawned the “Fit vs. Fat” studies.
Is Exercise Enough Without Weight Loss?
“So, I know being overweight isn’t healthy per se, but I work out a lot. Doesn’t that make a difference?”
Well, yes, but the difference depends on the context.
If you’re simultaneously fit but also have excess body fat, you’re said to be in a state of “fit fat.”
“Fit versus Fat” basically refers to the benefits of fitness being compared against the hazards of fatness.
In some cases, it’s more important that you be fit and body fat matters less, and in other cases the reverse is true.
Let’s look at a few cases where being fit is more important than not being fat.
Fitness vs. Fatness and Diabetes
Type ll diabetes occurs when insulin fails to properly deliver nutrients into muscle and fat cells; the two largest organs that are used as storage for glucose and other nutrients.
Well, exercise itself is able to improve the ability of both of these organs in handling glucose. A great review on how this happens is here (free to access), but the main takeaway is that exercise will independently improve handling of glucose and insulin sensitivity regardless of your body weight.
This may be more relevant to cardiovascular exercise than resistance training, and building and maintaining a good level of cardiovascular fitness reduces the risk of type II diabetes by itself.
Strength training also has its benefits, increasing insulin sensitivity and muscle mass; muscle mass by itself also has protective effects against developing diabetes in older and younger people.
Lifting some weights and then doing a bit of cardio afterwards, or doing workouts that improve both cardiovascular health and muscle mass (like interval training) is simply great even if fat is not lost.
For all intents and purposes, exercise alone is great for improving glucose handling and reducing the risk of developing diabetes even if you’re carrying a few extra pounds.
Fitness vs. Fatness and Cardiovascular Health
When you “get the blood pumping” with exercise it sort of implies that it would have a beneficial effect on cardiovascular health, which it does, but being obese is also considered a major risk factor for all-cause mortality related to heart issues.
Surprisingly, it’s not as clear cut as you would think.
When comparing those who identify as active versus those who identify as inactive, activity is associated with less risk, and if you had to choose between being “fit fat” or being “lean lazy” then “fit fat” does seem to be better.
While weight loss would benefit cardiovascular health, an active lifestyle does seem to partially protect against the negative effects of fat gain.
Fitness vs. Fatness and Mental Health
Exercise is sometimes recommended to keep the mind fresh and healthy, with recommendations ranging from just taking a simple walk in the morning to intense exercise.
When looking at older people, exercise does help protect brain health regardless of BMI. If you begin an exercise program for the purposes of improving brain function and reducing the risk of developing age-related diseases such as Alzheimer’s, then it looks like you don’t need to lose weight.
It would still be kind of nice though, as weight seems to be a risk factor for dementia . . .
If you just want to improve brain function and ward off brain-related diseases, exercise seems to be sufficient even if weight is not lost.
When Should You Lose Weight?
Truth be told, if you’re obese you should lose weight.
I know it’s tough, but when looking at everything we just talked about it’s pretty clear that:
- Being obese increases risk factors.
- Exercise reduces some, but not all, risk factors even when weight is not lost.
- Exercise paired with weight loss reduces most of these risk factors.
There are only two good reasons to stay obese: you prefer it that way (which is fine, you do you), or you have a specific medical condition that makes maintaining your current weight a better option at the moment; like increasing chances of survival while undergoing hemodialysis.
Hmm . . . I wonder what increased the risk of losing kidney function in the first place . . .
Anywho. From a strict health perspective, nobody should be in the obese range aside from people who know the risks and accept them, which is a tad bittersweet for me as long as you’re happy, or athletes who need to be at a high weight for their sport (sumo, American football, etc.)
There are some cases (most, in fact), where you absolutely should lose weight, like if you have the following goals.
You Need to Lose Weight if . . .
You Want to Live as Long As Possible
When it comes to maximizing longevity, it seems that being physically active isn’t enough.
Despite previous evidence on this topic suggesting that an elevated BMI was associated with protective effects, a follow-up analysis showed this was simply because many of the already sick people were at a low weight due to illness.
In other words, the advice of keeping a healthy BMI of around 18.5 to 25 still stands.
It’s not like being slightly over that guarantees you’ll die sooner, but it is significant. As the lead author puts it “ . . . an extra 3 to 4 units on the BMI scale is associated with a 5% increase in all cause mortality . . . ” So, going from a BMI of 20 to 23 to 24 increases your chances of dying over a set period of time by about 5 percent.
Also keep in mind this is a population based study using BMI as a measurement, and it may not apply (read: likely won’t apply) to situations where exercise is used to gain muscle mass while simultaneously losing fat mass.
Also don’t miss the forest for the trees here, it’s epidemiology.
A BMI of 25 may be an independent factor of all cause mortality but it’s not like exercise is irrelevant—it’s even more important—but if you want the best bang for your buck and the longest and healthiest life you can, let that exercise take a few pounds off as well.
For reducing your risk of dying, exercise. However, if you want the most benefits, exercise and get your BMI close to the normal, healthy range (maybe a bit above that if you have a lot of muscle mass). Don’t stay obese and think you’re fine.
You Need to Lose Weight if . . .
You Want to Sleep Well
Sleep apnea is a condition where breathing during sleep is interrupted.
Truth be told, there may be some instances where becoming physically fit helps sleep apnea even without any changes in weight, but other times sleep apnea is literally just the fault of being fat.
The reason is because if you’re lying on your back, excess weight on your chest can push down on your lungs, making it difficult to breath. This isn’t so much of an issue with being slightly overweight, but it becomes common for the obese.
This is a major reason why some people with sleep apnea choose to sleep in an upright position, and why weight loss itself can normalize breathing for about one in five people with sleep apnea who sleep on their backs.
If you have sleep apnea or other breathing issues during sleep (snoring), then you should strongly consider losing weight.
The Bottom Line on Fitness vs. Fatness
At the end of the day, being in the normal or overweight BMI range is ideal. Every instance of exercise benefiting health without weight loss is also an instance where weight loss would provide even more benefit.
But, weight loss is often hard and doesn’t happen as fast as we’d like, so it’s nice to know that not all efforts are futile. When it comes to maintaining your heart, brain, and metabolic health, being active is simply better than being inactive, regardless of your weight (although being leaner is still better).
That being said, this mainly applies to people who are overweight or obese. If you’re morbidly obese, then forget everything you read and get some protein powder and broccoli in you, start following a meal plan, and get in the gym.
What’s your take on being healthy if you’re overweight? Have anything else to share? Let me know in the comments below!
Scientific References +
- SA, J., JK, K., BA, E., SA, L., MT, N., JB, D., & GS, H. (2017). Improvement in Obstructive Sleep Apnea With Weight Loss is Dependent on Body Position During Sleep. Sleep, 40(5). https://doi.org/10.1093/SLEEP/ZSX047
- D, C., G, D. S., D, G., N, D., TIL, N., & P, R. (2018). Confounding by ill health in the observed association between BMI and mortality: evidence from the HUNT Study using offspring BMI as an instrument. International Journal of Epidemiology, 47(3), 760–770. https://doi.org/10.1093/IJE/DYX246
- G, D. S., JA, S., A, F., P, T., DA, L., & F, R. (2009). The association between BMI and mortality using offspring BMI as an indicator of own BMI: large intergenerational mortality study. BMJ (Clinical Research Ed.), 339(7739), 191. https://doi.org/10.1136/BMJ.B5043
- JL, L., MZ, M., A, N., MK, M., K, K.-Z., & CP, K. (2015). Association of age and BMI with kidney function and mortality: a cohort study. The Lancet. Diabetes & Endocrinology, 3(9), 704–714. https://doi.org/10.1016/S2213-8587(15)00128-X
- C, C., JP, G., A, D. B., S, C., P, P., & D, M. (2009). Is there any survival advantage of obesity in Southern European haemodialysis patients? Nephrology, Dialysis, Transplantation : Official Publication of the European Dialysis and Transplant Association - European Renal Association, 24(9), 2871–2876. https://doi.org/10.1093/NDT/GFP168
- M, K., R, L., GD, B., JE, F., J, P., ST, N., MJ, S., L, A., EI, F., M, G., A, K., M, K., E, K., M, N., SB, S., T, T., E, V., P, W., H, W., … M, J. (2018). Body mass index and risk of dementia: Analysis of individual-level data from 1.3 million individuals. Alzheimer’s & Dementia : The Journal of the Alzheimer’s Association, 14(5), 601–609. https://doi.org/10.1016/J.JALZ.2017.09.016
- MK, E., & PD, L. (2017). The fat-but-fit paradigm within the context of cognitive function. American Journal of Human Biology : The Official Journal of the Human Biology Council, 29(5). https://doi.org/10.1002/AJHB.23001
- E, F., & PD, L. (2017). Physical activity and cognitive function among older adults with hypertension. Journal of Hypertension, 35(6), 1271–1275. https://doi.org/10.1097/HJH.0000000000001311
- A, P., JD, B., & CJ, L. (2015). Cardiometabolic Disease Leading to Heart Failure: Better Fat and Fit Than Lean and Lazy. Current Heart Failure Reports, 12(5), 302–308. https://doi.org/10.1007/S11897-015-0265-5
- PD, L. (2016). The fat-but-fit paradigm and all-cause mortality among coronary artery disease patients. International Journal of Clinical Practice, 70(5), 406–408. https://doi.org/10.1111/IJCP.12799
- CC, K., MG, S., KH, L., S, S., J, H., GHH, T., K, G., YA, F., & NM, A. (2017). Association of BMI with risk of CVD mortality and all-cause mortality. Public Health Nutrition, 20(7), 1226–1234. https://doi.org/10.1017/S136898001600344X
- S, H., Y, C., HS, J., KE, Y., H, S., & S, R. (2017). Relative muscle mass and the risk of incident type 2 diabetes: A cohort study. PloS One, 12(11). https://doi.org/10.1371/JOURNAL.PONE.0188650
- JW, S., SS, L., SR, K., SJ, Y., BY, C., HY, S., & NH, C. (2017). Low muscle mass and risk of type 2 diabetes in middle-aged and older adults: findings from the KoGES. Diabetologia, 60(5), 865–872. https://doi.org/10.1007/S00125-016-4196-9
- GJ, V. D. H., ZJ, W., Z, C., G, T., E, M., PJ, S., & AL, S. (2010). Strength exercise improves muscle mass and hepatic insulin sensitivity in obese youth. Medicine and Science in Sports and Exercise, 42(11), 1973–1980. https://doi.org/10.1249/MSS.0B013E3181DF16D9
- H, M., SS, S., RA, S., Y, G., R, K., S, T., M, M., C, K., T, O., K, T., C, H., R, N., & SN, B. (2018). Importance of Achieving a “Fit” Cardiorespiratory Fitness Level for Several Years on the Incidence of Type 2 Diabetes Mellitus: A Japanese Cohort Study. Journal of Epidemiology, 28(5), 230–236. https://doi.org/10.2188/JEA.JE20160199
- DR, B. L., BV, R., C, P., TL, M., DE, K., TA, D., VW, D., JM, M., & M, S. (2017). Exercise-induced irisin release as a determinant of the metabolic response to exercise training in obese youth: the EXIT trial. Physiological Reports, 5(23). https://doi.org/10.14814/PHY2.13539
- Townsend, L. K., Knuth, C. M., & Wright, D. C. (2017). Cycling our way to fit fat. Physiological Reports, 5(7). https://doi.org/10.14814/PHY2.13247
- E, C., C, B., S, L., L, M., MC, P., M, T., MÈ, L., & V, P. (2017). A Health at Every Size intervention improves intuitive eating and diet quality in Canadian women. Clinical Nutrition (Edinburgh, Scotland), 36(3), 747–754. https://doi.org/10.1016/J.CLNU.2016.06.008
- JE, W., RJ, M., & CA, N. (2017). The Influence of Age the BMI and All-Cause Mortality Association: A Meta-Analysis. The Journal of Nutrition, Health & Aging, 21(10), 1254–1258. https://doi.org/10.1007/S12603-016-0837-4










